A comparative assessment of knee alignment and functional outcomes in total knee arthroplasty with mid vastus approach via computer-based hand-held navigation and conventional methods
2 Department of Orthopaedics, Basaveshwara Medical College and Research Centre, India, Email: ashishbc111@hotmail.com
Received: 19-Feb-2022, Manuscript No. jotsrr-21-50106; Editor assigned: 21-Feb-2022, Pre QC No. jotsrr-21-50106; Accepted Date: Feb 27, 2022 ; Reviewed: 24-Feb-2022 QC No. jotsrr-21-50106; Revised: 25-Feb-2022, Manuscript No. jotsrr-21-50106; Published: 28-Feb-2022, DOI: 10.37532/1897-2276.2022.17(1).64
This open-access article is distributed under the terms of the Creative Commons Attribution Non-Commercial License (CC BY-NC) (http://creativecommons.org/licenses/by-nc/4.0/), which permits reuse, distribution and reproduction of the article, provided that the original work is properly cited and the reuse is restricted to noncommercial purposes. For commercial reuse, contact reprints@pulsus.com
Abstract
Background: Total knee arthroplasty has greatly benefitted by the use of computer-aided navigation approaches. The latest chapter in the use of computer-aided devices in TKA is the application of accelerometer-based hand-held devices. With several advantages offered by the accelerometer-based navigation system, it is a promising candidate for preferred modality for TKA. The aim of this study is to compare the clinical, functional and radiological outcomes of accelerometer-based and conventional navigational approaches.
Methods: We assessed a total of 68 arthroplasties for comparison of pre-operative and post-operative parameters. For pre-operative outcomes we compared operative time and loss of blood/hemoglobin. For the post-operative outcomes, we considered the radiological outcomes used to assess optimum alignment, and used interviewer-administered International Knee Society’s functional and clinical Knee Society Score (KSS) and patient reported pain measured on Visual Acuity Score (VAS). The assessment of functional and clinical KS scores and pain (through VAS) was done one- and two-years post-surgery.
Results: Operative time is significantly higher in Accelerometer-Based Navigation (ABN) as compared to conventional method (p<0.000). Accelerometer-based navigation achieves better alignment of the implant as compared to conventional navigation (p<0.000, 0.001 and 0.017 in SFA, STA and FCA respectively and p<0.000 for post-operative mechanical axis). Patient-reported pain was significantly lower in the ABN group at two-year follow up (p=0.019). Investigator-assessed clinical and functional knee scores were also significantly higher in ABN group at the final follow-up (p=0.002 and 0.003 for clinical and functional scores, respectively). The difference in the functional (p=0.035) and clinical (p=0.023) knee scores within the groups pre- and post-operatively was also found to have changed significantly in the ABN group as compared to conventional group during the two-year follow up.
Conclusion: Better alignment, reduced number of outliers in terms of malalignment, better functional and clinical scores and reduced pain two-year post-surgery demonstrate the advantage of ABN approaches over conventional navigation. The higher operative times along with higher cost associated with ABN approach are the factors which might limit the expanse of ABN as the modality of choice.
Keywords
Total knee replacement, Accelerometer-based, Pain, Functional outcome, Knee score
Introduction
Several approaches have been used for Total Knee Arthroplasty (TKA) [1]. The procedure of TKA is undertaken to provide a stable, wellaligned knee joint and increase the quality of life of the patient. The minimally invasive, muscle sparing mid-vastus approach is widely used due to the advantages it offers over other approaches [2,3]. Ample alignment of the prosthesis, which is one of the prime factors governing the stability and function of the replaced knee, has been linked to loadbearing and survival of the implant. Survival of the implant has been shown to be affected if the coronal plane alignment is deviated beyond 0 ± 3° than the mechanical axis [4-8].
Computer-based assistance has been identified as a potent tool in orthopedic surgeries [9]. This approach has been widely used in TKAs because of its proposed and observed advantages over the conventional clinician-driven navigation approach [10-14]. When evaluated on terms of better radiological outcomes, Computer-Assisted Navigation (CAN) systems have been known to provide better spatial positioning of the implant and also improve biomechanics during walking [15- 17]. However, it is disputed whether CAN approaches can guarantee better functional outcomes, pain and quality of patients’ life over conventional clinician-based approach [18,19]. These functional and clinical outcomes have been assessed longitudinally between the two groups and the results have been predominantly inconclusive [20-24].
Although associated with better outcomes, there are certain disadvantages of using computer-based navigation systems [25]. Recent advent of accelerometer-based navigation devices have overcome the disadvantages of computer-based as well as conventional navigation systems, without compensating the accuracy or efficiency of either [26- 29].
The availability of studies that compare computer-assisted and clinician-based approaches in India, particularly on accelerometerbased navigation devices, is very limited if any [30]. Therefore, this study was undertaken to ascertain the difference in the radiological and functional outcomes of patients undergoing TKA with accelerometerbased handheld versus conventional navigation system in a tertiary care hospital in India.
Method
STUDY DESIGN
We conducted a prospective observational study over a period of two years, from April 2019 to May 2021. A total of 68 arthroplasties were completed in one and a half months and included in this study. Thirtysix arthroplasties were done via accelerometer-based navigation and 32 were conventional arthroplasties. Patients were followed up after one year and two-year from the date of surgery for assessment and scoring. The surgical procedures were carried out by a trained orthopedic surgeon.
PARTICIPANTS
All patients presenting in the orthopedic Out-Patient Department (OPD) with grade 4 knee osteoarthritis, irrespective of their gender, age and other anthropometric characteristics were included in the study. After providing information regarding the procedure and the modalities (conventional and computer-assisted) in a language of their understanding, patients were allowed to choose the modality of their choice and were requested to provide informed undersigned consent.
Patients were excluded if, they required simultaneous hip and knee arthroplasty were undergoing a revision knee surgery, had below knee or ankle deformity, had below knee or ipsilateral foot amputation or denied consent.
DATA COLLECTION
An independent physiotherapist from the hospital was allotted the task of measuring and recording anthropometric, clinical and study instrument-based data. The following tests were administered to the participants: International Knee Society Score (KSS)-functional and clinical, and Visual Analogue Score (VAS) for pain. All the data was collected and recorded in Microsoft Excel (Microsoft Corporation, USA).
SURGICAL APPROACH AND POST-OPERATIVE REHABILITATION
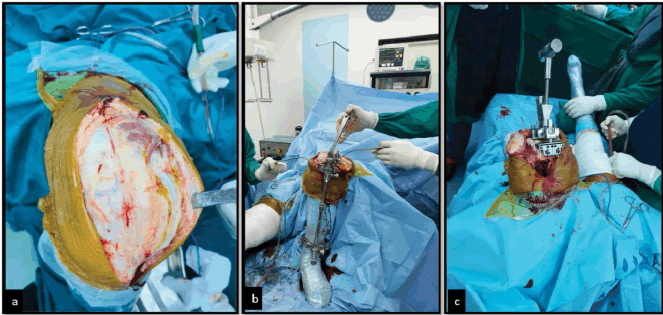
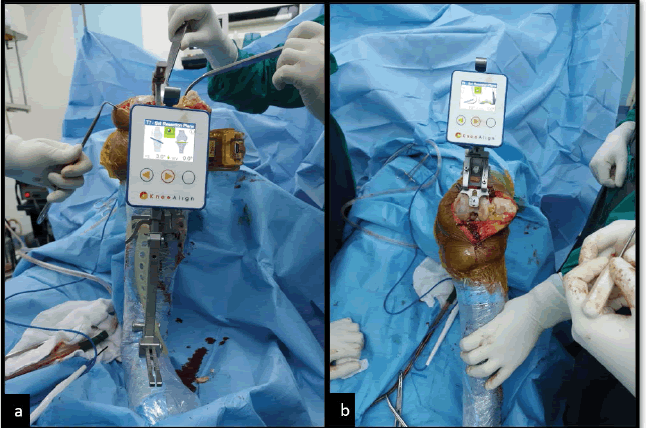
For the arthroplasty, quadriceps-sparing mid-vastus approach, first used by Engh (1997) [31] was adopted. An initial anterior midline incision was made, which was advanced to deep fascia via the subcutaneous tissue. This exposed the musculature of quadriceps. Vastus medialis was identified followed by blunt separation along its muscle fibers, to split the muscle in its full thickness. The incision was furthered distally along medial border of patella till the tibial tuberosity or as required for the surgery. Followed by division of the supra-patellar pouch, eversion and lateral dislocation of patella. After insertion of components and muscle fiber adaptation wound was closed in layers. Figures 1 and 2 demonstrate the surgical approaches undertaken and the instrumentation for both the arthroplasties. For rehabilitation, knee range of motion exercises were initiated on post-operative day one along with instructions for walking. On the 2nd post-operative day, the x-ray radiograph was obtained and bathroom training was started. Patients were discharged on 4th day after surgery and staples were removed on day 12.
Figure 1: Demonstration of conventional approach; a): Athrotomy carried out using the mid-vastus approach. This step was common for conventional and accelerometer-based navigation approaches; b): Tibial jig used during tibial resection in the conventional approach, and c): Femoral intramedullary jig used for taking distal femoral cuts in the conventional approach
OUTCOME MEASURES
Clinical and Radiological Outcomes: Duration of surgery, and pre- and post-operative hemoglobin (to assess drop in hemoglobin) were the clinical outcomes recorded.
Mechanical axis is defined as the line connecting the center of femoral head and mid-point of ankle joint, normally passing through the middle of the knee joint. For a knee to be considered well aligned, the mechanical axis must be close 180/0°.
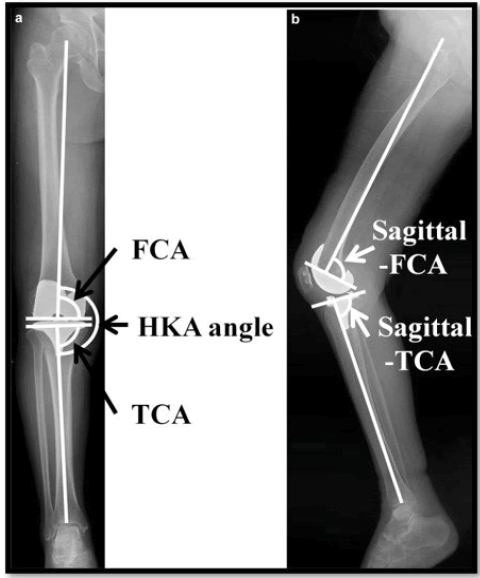
Assessment of Alignment: Alignment was assessed along the coronal and sagittal planes, using the following measures.
The angle between coronal femoral mechanical axis and inferior aspect of the femoral component known as the Femoral Component Angle (FCA) is measured as described earlier. Its alignment must be perpendicular to the mechanical axis in a well-aligned knee.
An angle measured between the sagittal mechanical femoral axis and a hypothetical line along posterior flange femoral component called sagittal femoral angle, and another angle called sagittal tibial angle measured between sagittal mechanical tibial axis and a hypothetical line along the proximal aspect of tibial component, are used to assess sagittal alignment.
Peri-operative aim was to achieve a sagittal alignment with a flexion of three degrees of femoral prosthesis with respect to axis of femur and a posterior slope of three degrees of tibial prosthesis with respect to axis of tibia.
Radiological Imaging: The post-operative radiographic evaluation was done one day after removal of drain. This included X-ray imaging and goniometric assessment. For this purpose, a series of lateral views-in full extension, at 45° and 90° flexion and in full flexion-of the knee were obtained under unipodal weight bearing condition to assess sagittal mobility. A forced valgus view to assess the height of the lateral compartment, an anteroposterior view to detect any medial overhang.
For measurement of mechanical axis, full length (hip to ankle) weight bearing x-ray radiograph with knee flexion of 20° was obtained at a dose of 0.01 mSv was obtained in anteroposterior view. Radiographic measurements were done using the DICOM viewer software Oviyam 2.0 and angles were measured up to one decimal place.
Assessment of Knee Condition: The condition of individual knee was assessed pre- and post-operatively using the Knee Society Score (KSS) on the functional and clinical domains. The individual functional and clinical scores are calculated out of 100, the condition of the knee is directly proportional to the score. The functional and clinical KS Scores were assessed one year after the date of surgery.
Patient Reported Outcome: The patient perceived chronic and acute pain was measured and recorded using the Visual Analogue Score (VAS). The pain intensity gets higher as the values on VAS scale get higher.
STATISTICAL ANALYSIS
All the statistical analyses were carried out using IBM-SPSS version 26 (New York, USA). The data was first tested for normal distribution by Kolmogorov-Smirnov test. Descriptive variables are expressed as mean and standard deviation, and frequencies. Mann-Whitney U test was used to compare the data of the two groups for continuous variables. A p-value of <0.05 was considered to be statistically significant.
Post-hoc power analysis was conducted to assess the power of the study using G* power (v 3.1.9.4) software [32]. With an effect size of 0.5 and type-I error probability of 0.05, 68 number of participants in the current study, a power of 0.98 is obtained.
Results
PATIENT CHARACTERISTICS
A total of 60 patients were recruited for the study. Of these 60, 31 patients underwent conventional TKR, whereas, 29 patients underwent computer-assisted accelerometer-aided TKR. One patient in the conventional group and six patients in the computer-assisted group underwent bilateral TKR. Thus, a total of 68 knees (40 right and 28 left) were operated up on and followed-up during the study period. The number of knees operated by conventional method was 36 and those operated by accelerometer-based system was 32.
Baseline characteristics of the participants, namely, age, gender, knee, height, weight and BMI are enlisted in Table 1. There was no significant difference in the baseline characteristics of the patient in the two groups.
Table 1. Demographic details of the sample (mean and standard deviation)
| S. No. | Demographics | Total (n=68) | Computer-assisted navigation group (n=36) | Conventional group (n=32) | p-value |
|---|---|---|---|---|---|
| 1 | Age (years) | 62.78±6.2 | 62.28±6.1 | 63.34±6.3 | 0.134 |
| 2 | Gender (n) | M: 25 | M: 10 | M: 15 | 0.106 |
| F: 43 | F: 26 | F: 17 | |||
| 3 | Knee (n) | R: 40 | R: 21 | R: 19 | 0.931 |
| L: 28 | L: 15 | L: 13 | |||
| 4 | Height (m) | 1.63±0.07 | 1.64±0.06 | 1.62±0.08 | 0.187 |
| 5 | Weight (kg) | 80.38±9.31 | 80.55±10.7 | 80.18±7.5 | 0.768 |
| 6 | BMI | 29.93±3.39 | 29.93±3.39 | 29.93±3.39 | 0.576 |
OUTCOME MEASURES
Clinical and Peri-Operative Measures and Post-Operative Outcomes: Difference in the mean duration of surgery between the two groups was statistically significant (p<0.000). Other clinical outcome, pre- and post-operative hemoglobin levels were not statistically different (Table 2). A total of 14 patients (7 from each group) required transfusion (p=0.809). The difference in peri-operative measures of SFA (p<0.000), STA (p=0.001) and FCA (p=0.017) were statistically significant across the two groups. Although there was no significant difference between the pre-operative mechanical axis (p=0.68), the post-operative mechanical axis was significantly different (p<0.000). These and other outcome variables are tabulated in Tables 2 and 3. Figure 3 shows the radiographs used for assessment of radiological parameters.
Table 2. Pre-operative and post-operative parameters (mean and standard deviation)
| S. No. | Parameter | Total (n=68) | Computer-assisted navigation group (n=36) | Conventional group (n=32) | p-value |
|---|---|---|---|---|---|
| 1 | Duration of surgery (minutes) | 75.79±10.32 | 80.42±9.93 | 70.59±11.11 | <0.000 |
| 2 | Hemoglobin-Pre-Operative | 11.22±1.13 | 11.16±1.19 | 11.28±1.07 | 0.61 |
| 3 | Hemoglobin-Post-Operative | 9.52±1.35 | 9.53±1.4 | 9.51±1.33 | 0.84 |
| 4 | Femoral Component Flexion Angle (FCA) | 91.92±1.04 | 91.59±0.79 | 92.29±1.17 | 0.017 |
| 5 | Sagittal Femoral Component Angle (SFA) | 90.40±1.62 | 89.32±0.76 | 91.61±1.48 | <0.000 |
| 6 | Sagittal Tibial Component Angle (STA) | 84.71±0.80 | 84.41±0.75 | 85.04±0.74 | 0.001 |
| 7 | Mechanical axis-pre-operative | 166.54±1.9 | 166.63±2.11 | 166.43±1.88 | 0.905 |
| 8 | Mechanical axis-post-operative | 178.39±1.27 | 178.97±1.25 | 177.75±0.95 | <0.000 |
| 9 | KSS-Clinical Score-Pre-operative | 32.59±10.5 | 31.25±10.7 | 34.09±10.3 | 0.38 |
| 10 | KSS-Clinical Score-1 year | 84.06±5.75 | 86.64±5.5 | 81.16±4.4 | <0.000 |
| 11 | KSS-Clinical Score-2 year | 91.07±5.36 | 92.81±3.27 | 89.12±4.65 | 0.002 |
| 12 | KSS-Functional Score-Pre operative | 50.09±26.23 | 56.56±26.03 | 42.81±24.88 | 0.012 |
| 13 | KSS-Functional Score-1 year | 91.85±8.67 | 96.39±4.8 | 86.75±9.2 | <0.000 |
| 14 | KSS-Functional Score-2 year | 98.49±2.35 | 99.31±1.7 | 97.56±2.62 | 0.003 |
| 15 | VAS- Preoperative | 8.68±0.76 | 8.56±0.90 | 8.81±0.5 | 0.21 |
| 16 | VAS- Post operative | 1.22±0.51 | 1.36±0.63 | 1.06±0.24 | 0.019 |
| 17 | Need for transfusion (n, %) | 14 (20.6) | 7 (19.4) | 7 (21.9) | 0.809 |
KSS clinical and functional scores were found to be statistically significant at both; one-year and two-year follow ups across the two groups (Table 2).
Patient-reported outcome: Difference in VAS scores was statistically significant in the one- and two-year post-operative follow-up (Table 2).
Difference in Pre-Operative and Post-Operative Clinical, Radiological and Patient Reported Outcomes: Although the drop in hemoglobin (p=0.52) was not different among the two groups, the difference in change of mechanical axis (p=0.045) was statistically significant. Among other outcomes, difference KSS clinical score was significantly different in the two groups at one year (p=0.015) and two years after the surgery (p=0.035). The KSS functional score was found to be significant at the two year follow up (p=0.023) (Table 3).
Table 3. Difference in pre- and post-operative outcome parameters (means and standard deviations)
| S. No. | Difference in Parameters (Pre-operative value-Post-operative value) | Total (n=68) | Computer-assisted navigation group (n=36) | Conventional group (n=32) | p-value |
|---|---|---|---|---|---|
| 1 | Hemoglobin | -1.69±0.87 | -1.62±0.85 | -1.76±0.91 | 0.6 |
| 2 | Mechanical Axis | 11.85±2.20 | 12.33±2.41 | 11.31±1.82 | 0.045 |
| 3 | KSS Clinical Score (1 year) | 51.47±12.10 | 55.38±12.96 | 47.06±9.44 | 0.005 |
| 4 | KSS Clinical Score (2 year) | 58.49±11.21 | 61.56±11.50 | 55.03±9.94 | 0.035 |
| 5 | KSS Functional Score (1 year) | 41.76±21.25 | 39.83±23.24 | 43.93±18.89 | 0.5 |
| 6 | KSS Functional Score (2 year) | 48.40±25.21 | 42.75±25.41 | 54.75±23.78 | 0.023 |
| 7 | VAS | -7.45±0.95 | -7.19±1.16 | -7.75±0.50 | 0.04 |
Discussion
This study revealed that knees operated with Accelerometer-Based Navigation (ABN) approach have better radiological alignment, better clinical outcome and decreased pain, at the one-year and subsequent two-year follow-up. The outcomes were measured using mechanical alignment measurements and alignment angles (FCA, SFA and STA) for radiological outcomes, KSS for functional and clinical outcomes and VAS for the patient-reported outcome. Computer-assisted accelerometer-based TKA has become increasingly common in the recent past. Although associated with increased duration of surgery, computer-assisted surgeries are expected to offer several advantages over clinician’s assessment [12].
The mean duration of surgery with the ABN is significantly higher than conventional navigation (Table 2). This is similar and comparable to the findings by Liow et al and Denti et al. [33,33] Although there might be studies that argue otherwise but our study is consistent with the overall evidence [35,36]. Optimum knee alignment is the primary aim of TKA. In our study all the radiological outcomes established that ABN was significantly superior in achieving better alignment than conventional approach. There exists literature which shows that both approaches show similar outcomes [34,37]. Results of our study are similar to several previous studies where the superiority of ABN has been underlined through a variety of studies, including retrospective studies, randomized controlled trials and meta-analyses [33,35,38-42]. Accelerometer-based navigation group achieved a significantly better overall alignment (mechanical axis) as compared to the conventional group. The change in pre- and post-operative mechanical axis in our study was also found to be statistically significant with magnitude of change being more (and desirable) in ABN group. In our study, the malalignment (>3º) was only found in the conventional approach group and the degree of alignment between the two groups is also significantly different (p<0.000).
One of the advantages of computer-assisted surgeries is lesser blood loss. In our study the difference in blood loss and the need of transfusion was not found to be significantly different for both the groups. As per the recommendations of previous studies where various risk factors associated with blood loss during TKA are analyzed [30,43] hidden blood loss must be considered in addition to transfusion. In our study, it was found that the loss of hemoglobin, in addition to transfusion needs, was not significantly different in the two groups, and none of the patients suffered from post-operative anemia. These findings are similar to a previous study safety of CAN systems is discussed [37].
Obesity is one of the many factors that influence the need and success of TKA. In our study it was found that there was no effect of obesity on knee alignment and other outcomes in the two groups, supported by other previous studies [35].
The difference between pre-operative and one-year and two-year follow-up functional and clinical KS scores was significant between the two groups, with ABN group attaining significantly higher scores as compared to conventional group. Several studies have demonstrated that [36,40-42,44] despite better radiological outcomes and alignments, computer-assisted hand held navigation and conventional approaches yield same results in terms of functional outcomes of the patients. Our findings are similar to another study where the authors have reported a significant change in KSS in the ABN group. Furthermore, the difference in the clinical scores at one year follow-up was also statistically significant. Although not significant, the change in the KS functional score in the two groups was also higher in ABN. Moreover, the difference in the clinical and functional scores between the two groups at two-year follow-up was statistically significant. These findings support the significance of accelerometer-based approach over others.
Subjective measurement of pain was also compared between the two groups. Pain reduction was significantly higher in the ABN group as ascertained by comparing the VAS scores at one year follow-up and the change in VAS score pre- and post-operatively. This finding is similar to another single surgeon study where 52 patients were followed up and assessed after 6 months of arthroplasty. [45] The findings of our study contrast with the result of previous studies where patient-reported outcomes were shown to be comparable and not significantly different in the two groups [20,21,46].
The primary aim of any joint replacement surgery is to attain optimum limb function and improve the quality of life of the patients. In these terms our study clearly demonstrates the advantages offered by the accelerometer-based navigation approach over the conventional clinician governed navigation. Although, the duration of surgery is longer than in the conventional approach. It is systemic to computerbased navigation systems, and comparatively accelerometer-based navigation requires lesser time. It also requires lesser manpower than conventional navigation and is easily manipulable with a handheld device rather than other elaborate computer-bases systems. The system, however, offers no advantage in terms of decreased blood loss or for obese patients, over the conventional system.
The strength of this study is assessment of objective and subjective outcomes after one and two years of the surgery, in addition to radiological outcomes. Both the assessments revealed that the improvement in accelerometer-based navigation was significantly higher than the improvement in conventional navigation. Thus, this study provides more evidence to clinicians and academicians to assess the suitability and use of accelerometer-based approaches. The limitation of this study is the limited sample size which can be addressed in the future studies. Another factor to be considered is the long-term outcomes of accelerometer-based navigation on functional outcomes of TKR. The current study clearly demonstrates the efficacy of ABN approach over the conventional one in intermediate temporal frame. This will make decision-making in a resource-limited setting, such as India, easier. Another important factor that needs to be mentioned is the affordability of ABN approach as the cost of such surgeries are higher than conventional, owing to requirement of trained surgeon and instrumentation.
Conclusion
Use of accelerometer-based navigation system in TKA provides better alignment of the implant and better clinical and functional outcomes two years after the surgery, with mild increment in the duration of surgery. Subsequent longer-term follow-ups will reveal definitive superiority of ABN system in implant survival and functional outcomes over other approaches.
REFERENCES
- Liu H.W., et al.: Surgical approaches in total knee arthroplasty: a meta-analysis comparing the midvastus and subvastus to the medial peripatellar approach. J Arthroplasty. 2014;29:298-304.
- Hube R., Sotereanos N.G., Reichel H.: The midvastus approach for total knee arthroplasty. Orthop Traumatol. 2002;10:235-244.
- Engh GA.: Surgical technique of the midvastus arthrotomy. Clin Orthop. 1998;351:270-274.
- Lotke P.A., Ecker M.L.: Influence of positioning of prosthesis in total knee replacement. J Bone Joint Surg Am. 1977;59:77-79.
- Ritter M.A., et al.: Postoperative alignment of total knee replacement: its effect on survival. Clin Orthop. 1994;299:153-156. Google Scholar]
- Abdel M.P., et al.: Effect of postoperative mechanical axis alignment on survival and functional outcomes of modern total knee arthroplasties with cement: a concise follow-up at 20 Years. JBJS. 2018;100:472-478.
- Hsu RW, Himeno S, Coventry MB, Chao EY. Normal axial alignment of the low er extremity and load-bearing distribution at the knee. Clin Orthop. 1990;255:215-227.
- Morgan S.S., et al.: The influence of postoperative coronal alignment on revision surgery in total knee arthroplasty. Int Orthop. 2008;32:639-642.
- Pearle A.D., Kendoff D., Musahl V.: Perspectives on computer-assisted orthopaedic surgery: movement toward quantitative orthopaedic surgery. J Bone Joint Surg Am. 2009;91:7-12.
- Anderson K.C., Buehler K.C., Markel D.C.: Computer assisted navigation in total knee arthroplasty: comparison with conventional methods. J Arthroplasty. 2005;20:132-138.
- Hernigou J., Morel X., Hernigou P.: Computer navigation technique for simultaneous total knee arthroplasty and opening wedge high tibial osteotomy in patients with large tibial varus deformity. Surg Technol Int. 2020;37:265-274.
- Gothesen O., et al.: Computerized navigation: a useful tool in total knee replacement. JBJS Essent Surg Tech. 2020;10:e0022. Google Scholar]
[CrossRef]
- Ayekoloye C., Nwangwu O., Alonge T.: Computer navigation-assisted knee replacement demonstrates improved outcome compared with conventional knee replacement at mid-term follow-up: a systematic review and meta-analysis. Indian J Orthop. 2020;54:757-766.
- Jenny J.Y., Boeri C.: Computer-assisted implantation of total knee prostheses: a case-control comparative study with classical instrumentation. Comput Aided Surg Off J Int Soc Comput Aided Surg. 2001;6:217-220.
- Bauwens K., et al.: Navigated total knee replacement: a meta-analysis. J Bone Joint Surg Am. 2007;89:261-269.
- Matziolis G., et al.: A prospective, randomized study of computer-assisted and conventional total knee arthroplasty: three-dimensional evaluation of implant alignment and rotation. JBJS. 2007;89:236-243.
- McClelland J.A., et al.: Total knee arthroplasty with computer-assisted navigation more closely replicates normal knee biomechanics than conventional surgery. The Knee. 2017;24:651-.656.
- Dyrhovden G.S., et al.: Is the use of computer navigation in total knee arthroplasty improving implant positioning and function? A comparative study of 198 knees operated at a Norwegian district hospital. BMC Musculoskelet Disord. 2013;14:321.
- Hsu R.W., et al.: Comparison of computer-assisted navigation and conventional instrumentation for bilateral total knee arthroplasty: The outcomes at mid-term follow-up. Medicine (Baltimore). 2019;98:e18083.
- Singisetti K., et al.: Navigation-assisted versus conventional total knee replacement: no difference in patient-reported outcome measures (PROMs) at 1 and 2 years. Arch Orthop Trauma Surg. 2015;135:1595-1601.
- Kamat Y.D., et al.: Does computer navigation in total knee arthroplasty improve patient outcome at midterm follow-up? Int Orthop. 2009;33:1567-1570.
- Lüring C., et al.: A five to seven year follow-up comparing computer-assisted vs freehand TKR with regard to clinical parameters. Int Orthop. 2012;36:553-558.
- Ishida K., et al.: Mid-term outcomes of computer-assisted total knee arthroplasty. Knee Surg Sports Traumatol Arthrosc. 2011;19:1107-1112.
- Parratte S., et al.: Effect of postoperative mechanical axis alignment on the fifteen-year survival of modern, cemented total knee replacements. J Bone Joint Surg Am. 2010;92:2143-2149.
- Cozzi Lepri A., et al.: Accelerometer-based navigation in total knee arthroplasty for the management of extra-articular deformity and retained femoral hardware: analysis of component alignment. Joints. 2019;7:1-7.
- Goh G.S.H., et al.: Accelerometer-based navigation is as accurate as optical computer navigation in restoring the joint line and mechanical axis after total knee arthroplasty: a prospective matched study. J Arthroplasty. 2016;31:92-97.
- Nam D., et al.: Accelerometer-based, portable navigation vs imageless, large-console computer-assisted navigation in total knee arthroplasty: a comparison of radiographic results. J Arthroplasty. 2013;28:255-261.
- Nam D., et al.: Accelerometer-based computer navigation for performing the distal femoral resection in total knee arthroplasty. J Arthroplasty. 2012;27:1717-1722.
- Gao X., et al.: Comparison of the accelerometer-based navigation system with conventional instruments for total knee arthroplasty: a propensity score-matched analysis. J Orthop Surg. 2019;14:223.
- Singla A., et al.: A randomized controlled study to compare the total and hidden blood loss in computer-assisted surgery and conventional surgical technique of total knee replacement. Clin Orthop Surg. 2015;7:211-216.
- Engh G.A., Holt B.T., Parks N.L.: A midvastus muscle-splitting approach for total knee arthroplasty. J Arthroplasty. 1997;12:322-331.
- Faul F., et al.: G*Power 3: a flexible statistical power analysis program for the social, behavioral, and biomedical sciences. Behav Res Methods. 2007;39:175-191.
- Liow M.H.L, et al.: Computer-assisted stereotaxic navigation improves the accuracy of mechanical alignment and component positioning in total knee arthroplasty. Arch Orthop Trauma Surg. 2016;136:1173-1180.
- Denti M., et al. Conventional versus smart wireless navigation in total knee replacement: similar outcomes in a randomized prospective study. Joints. 2018;6:90-94.
- Thiengwittayaporn S., et al.: Hand-held navigation may improve accuracy in minimally invasive total knee arthroplasty: a prospective randomized controlled trial. Int Orthop. 2016;40:51-57.
- Li J.T., Gao X., Li X.: Comparison of iASSIST navigation system with conventional techniques in total knee arthroplasty: a systematic review and meta-analysis of radiographic and clinical outcomes. Orthop Surg. 2019;11:985-993.
- Moo I.H., et al.: Similar radiological results with accelerometer-based navigation versus conventional technique in total knee arthroplasty. J Orthop Surg Hong Kong. 2018;26:2309499018772374.
- Kinney M.C., et al. Comparison of the iAssist handheld guidance system to conventional instruments for mechanical axis restoration in total knee arthroplasty. J Arthroplasty. 2018;33:61-66.
- Rhee S.J., et al. A comparison of long-term outcomes of computer-navigated and conventional total knee arthroplasty: a meta-analysis of randomized controlled trials. J Bone Joint Surg Am. 2019;101:1875-1885.
- Selvanayagam R., et al.: A prospective randomized study comparing navigation versus conventional total knee arthroplasty. J Orthop Surg Hong Kong. 2019;27:2309499019848079.
- Petursson G., et al.: Computer-assisted compared with conventional total knee replacement: a multicenter parallel-group randomized controlled trial. J Bone Joint Surg Am. 2018;100:1265-1274.
- Lee D.Y., et al.: No differences in mid- to long-term outcomes of computer-assisted navigation versus conventional total knee arthroplasty. Knee Surg Sports Traumatol Arthrosc Off J ESSKA. 2020;28:3183-3192.
- Prasad N., Padmanabhan V., Mullaji A.: Blood loss in total knee arthroplasty: an analysis of risk factors. Int Orthop. 2007;31:39-44.
- Matsumoto T., et al.: Current concepts and future perspectives in computer-assisted navigated total knee replacement. Int Orthop. 2019;43:1337-1343.
- Peterlein C.D., et al. Clinical outcome and quality of life after computer-assisted total knee arthroplasty: results from a prospective, single-surgeon study and review of the literature. Musculoskelet Surg. 2009;93:115.
- Hernández-Vaquero D., Suarez-Vazquez A., Iglesias-Fernandez S.: Can computer assistance improve the clinical and functional scores in total knee arthroplasty? Clin Orthop. 2011;469:3436-3442.



 Journal of Orthopaedics Trauma Surgery and Related Research a publication of Polish Society, is a peer-reviewed online journal with quaterly print on demand compilation of issues published.
Journal of Orthopaedics Trauma Surgery and Related Research a publication of Polish Society, is a peer-reviewed online journal with quaterly print on demand compilation of issues published.