A rare localization of tuberculosis in sternoclavicular joint: A rare uncommon manifestation of extrapulmonary disease recovered in government medical teaching institute of middle India
Received: 12-Jun-2020 Accepted Date: Jul 22, 2020 ; Published: 30-Jul-2020
This open-access article is distributed under the terms of the Creative Commons Attribution Non-Commercial License (CC BY-NC) (http://creativecommons.org/licenses/by-nc/4.0/), which permits reuse, distribution and reproduction of the article, provided that the original work is properly cited and the reuse is restricted to noncommercial purposes. For commercial reuse, contact reprints@pulsus.com
Abstract
Tuberculosis (TB) is still a very common disease in developing countries. Primary tuberculosis of the sternoclavicular joint is an extremely rare disease caused by Mycobacterium tuberculosis bacillus. Diagnosis was arrived at by clinical, radiological, and microscopic examinations. Diagnosis is usually based on demonstration of granulomas on histopathology. Good radiographs and imaging studies are supportive for diagnosis. Early diagnosis and prompt treatment with standard drug regimen of Anti-Tubercular Therapy (ATT) would hasten complete recovery. Here we are reporting 9 cases who presented with swelling of sternoclavicular joint with non-specific signs and symptoms later diagnosed to be a case of sternoclavicular joint tuberculosis. Patients were treated and cured with antitubercular regimen.
Keywords
tuberculosis, sternoclavicular joint, TB arthritis, musculoskeletal system
Introduction
Tuberculosis TB arthritis is seen among children and young adults in endemic regions of the developing countries [1] whereas in the developed countries it is seen in the older population and immunocompromised patients. Musculoskeletal system tuberculosis can occur due to the dissemination of pulmonary tuberculosis or as a primary disease [1]. Musculoskeletal system tuberculosis mostly affects the spinal vertebrate, hip, knee, wrist and very rarely the thoracic cage (1% to 5%). TB of the sternoclavicular joint occurs due to reactivation of latent infection was diagnosed and the patient was started on Category 1 antitubercular therapy the diagnosis can be done by pain and swelling, ruptured abscesses and serial radiographs along with culture and sensitivity.
Patient and Methods
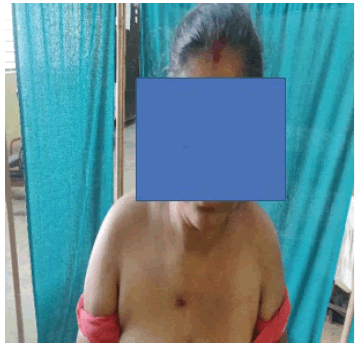
The study was conducted between 2018 to 2020 in central India Government Medical Teaching Institute, Rewa of Madhya Pradesh, India. There were 9 patients came with tubercular arthritis of sternoclavicular joint their mean age was 43 (30-55) years in which number of male (n=6) and female (n=3). In which right side involvement is (n=7), the left side is (n=2). Initially there was painless swelling of the right sternoclavicular joint (Fig. 1) with discharging sinus (n=3) and there was swelling which was gradually increasing in size and was accompanied with pain (n=6). There were 2 patients who was suffering from ankylosing spondylitis and diabetes mellitus type 2. There were constitutional symptoms such as weight loss and low-grade fever in 3 patients for past 7 months. There was no previous history of tuberculosis or contacted with open case of tuberculosis [2].
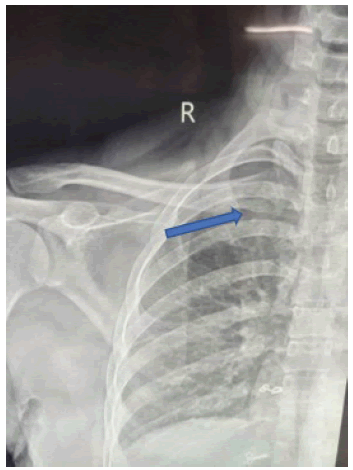
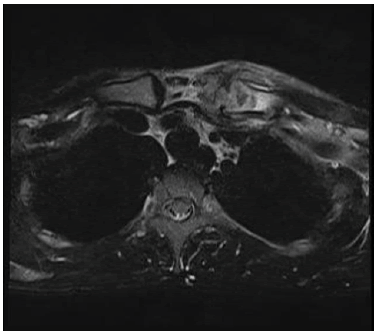
Laboratory hematological test reveals increase in leukocyte and Erythrocyte Sedimentation Rate (ESR). There is negative in HIV tests. No cervical and axillary lymphadenopathy. There was discharging sinus 3 patients in which immediately sent for culture and sensitivity. FNAC was done in every patient in which there was evidence of granulomatous pathology. Mantoux test was done in every patient which was positive. All patients had a positive culture and sensitivity for acid-fast bacilli were shown (Fig. 1). Plain radiographs show doubtful cystic lesion in the medial end of clavicle in 2 patients others were unremarkable in all cases (Fig. 2). MRI was performed in 3 cases there was granulation/ abscess formation in the soft tissue adjacent to right sternoclavicular joint and medial side of right clavicle (Fig. 3).
All the patients were started with anti-tubercular regimen including four drugs category 1 that is (HRZE)-isoniazid (300 mg) daily, rifampicin (450 mg), pyrazinamide (1000-1500 mg), ethambutol (800 mg) daily associated with vitamin B complex. All drugs were continued for 12 months-14 months later on depending upon clinical response of treatment and erythrocyte sedimentation rate value decreasing type two drugs were omitted initially that was pyrazinamide and ethambutol [1-3]. So, isoniazid and rifampicin were continued as a maintenance therapy. In (case-4,6,9) ATT was continued till 20 months due to delayed in evidence of healing.
MRI showing granulation/abscess formation in the soft tissue adjacent to right sternoclavicular joint and medial side of right clavicle (Table 1).
| Case number | Age/sex | Chief complaints | diagnosis | Other diseases | Treatment | Recover period | Sternoclavicular joint side |
|---|---|---|---|---|---|---|---|
| Case 1 | 35/female | Discharging sinus for 5 days | AFB-ZN stain with Mantoux test positive | No | ATT | 18 months | Right |
| Case 2 | 43 years/female | Pain and swelling for 2 months | AFB-ZN stain with Mantoux test positive | Ankylosing spondylitis | ATT | 14 months | Right |
| Case 3 | 36 years/male | Discharging sinus | Epithelioid cells with caseating granulomatous lesion in biopsy | No | ATT | 16 months | Right |
| Case 4 | 49 years/female | Pain and swelling for 3 months | AFB-ZN STAIN with Mantoux test positive | Diabetes mellitus type 2 | ATT | 20 months | Right |
| Case 5 | 31 years/male | Pain and swelling for 6 months | Epithelioid cells with caseating granulomatous lesion in biopsy | No | ATT | 16.7 months | Right |
| Case 6 | 48 years/male | Pain and swelling for 4 months | AFB-ZN stain with caseating granulomatous lesion in biopsy | No | ATT | 20 months | Right |
| Case 7 | 53 years/male | Pain and swelling for 7 months | AFB-ZN stain with Mantoux test positive | No | ATT | 16 months | Right |
| Case 8 | 37 years/male | Pain and swelling 9 months | AFB-ZN stain with Mantoux test positive | No | ATT | 18 months | Left |
| Case 9 | 55 years/male | Painless discharging sinus for 9 months | AFB- ZN stain with Mantoux test positive | No | ATT | 21 months | Left |
| AFB: Acid Fast Bacilli; ZN stain: Zeihl-Neelsen; ATT: Anti Tubercular Treatment | |||||||
Table 1. Patients characteristics and content
Discussion
TB has always remained a significant infection in developing countries. There are a number of clinical and radiographic features of osseous TB, which mimics a wide range of pathologies, hence, the involvement of extrapulmonary features can be particularly difficult to diagnose.
The final diagnosis was arrived at in these cases on the basis of clinical examination, suspicious radiographs, and representative tissue biopsy. Differential diagnoses linked, such as subacute or chronic suppurative arthritis, rheumatoid arthritis, benign bone tumors, osteochondrosis, and Kaposi sarcoma, which further makes it difficult to come to a conclusive diagnosis [4]. In case of TB of sternoclavicular joint early diagnosis is essential to prevent further complication including migration of abscesses in the mediastinum region. The lesion also can be misdiagnosed as chronic osteomyelitis as presented by this case in which bone destruction is present. On review, the chief presenting complaints were swelling, pain, fever, discharging sinuses or a combination of these. On examination, the joint is usually minimally tender in early stages with non-pulsatile swelling without raised temperature of the skin. Fever was present in six cases which was much less than the expected. Discharging sinuses were an uncommon symptom with only three cases presented with it.
In the present study also, it was observed that pain and swelling are the most common symptoms in six patients associated with diabetes mellitus and ankylosing spondylitis in two patients who are immune compromised. Only one of our patients had swelling without pain and two patients had pain without any obvious swelling.
Today there are more than 30 literatures present in which most of cases pain and swelling with mild rise of temperature is common symptoms. Kumar S, Jain VK, Sternoclavicular joint tuberculosis: A series of conservatively managed sixteen cases, Shah reported 8 cases of SCJ TB, in which they noticed pain, swelling and fever to be the most common symptom combination (6 out of 8) [4]. Dhillon et al. in their study of 9 cases, also reported pain and swelling as common symptoms [4-6].
In our study we have found tuberculosis is most common in developing countries in which middle age men are involved. Total nine cases are involved in which common complaints are pain, swelling and discharging sinus. We observed that pain associated with swelling other discharging sinus associated with joint destruction associated with constitutional symptoms [6]. Fine-needle aspiration biopsy was performed in every patient and open biopsy was performed in 2 patients where Fine-Needle Aspiration Cytology (FNAC) was nonconclusive. Evidence of caseous granulomatous pathology was obtained in every case. Acid-fast bacilli was seen after Ziehl-Neelsen staining was done. After confirmation of diagnosis, all the patients were put on an antitubercular regimen (Antitubercular Therapy-ATT) consisting of four drugs-rifampicin (10 mg/Kg daily), isoniazid (5 mg/Kg daily), ethambutol (15 mg/Kg daily) and pyrazinamide (25 mg/Kg in divided doses)-in the initial intensive phase for 10-12 months. After that, depending on the clinical response to treatment, patients were switched over to three drugs (isoniazid, rifampicin and ethambutol), followed 1 or 2 months later by the omission of ethambutol [7]. Isoniazid and rifampicin were continued as maintenance therapy for 14-21 months. Final outcome of therapy was judged by clinical, hematological, and radiological parameters were obtained.
Tuberculosis can affect almost any part of the body due to the advent of multidrug resistant strains of Mycobacterium tuberculosis and acquired immunodeficiency syndrome. Approximately 1% of musculoskeletal system tuberculosis occurs in the sternum and sternoclavicular region. It is thought to be caused by either reactivation or spreading of the foci of tubercle bacilli through hematogenous/lymphatic spread or by direct extension from lung or pleura. Tuberculosis of Sternoclavicular joint is often diagnosed late or misdiagnosed due to absence of constitutional symptoms, unusual site and indolent nature of the disease. TB of the SC joint may follow a more aggressive leading to a painful, destroyed joint or a slowly progressive, relatively painless disease without constitutional symptoms and minimal joint destruction due to differences in the virulence of the organisms and host resistance. The patients may present with painful or painless swelling and very rarely with sinus. In our study 6 patients had painless swelling and 3 had painless swelling along with a discharging sinus. Constitutional symptoms like fever and weight loss was seen in 5 patients.
Conventional plain radiographs are not helpful in diagnosing this pathology. CT and MRI can be used. In a study done by Shah [4] suggested that all radiological and imaging modalities are complementary but MRI is the best technique for early detection and diagnosis of SC joint TB [4]. MRI shows the spread in the medulla of the bone and involvement in the soft tissue better in our case, an abscess was seen in medial end of right clavicle and right side of sternum adjacent to right sternoclavicular joint [8-10].
The final histological and microbiological confirmation of SC joint TB requires detection of tubercle bacilli in tissue culture or showing caseous granulomas or detecting AFB in biopsy. In cases where the diagnosis cannot be made, bacterial DNA detection can be carried out with Polymerase Chain Reaction (PCR) from infected tissue specimens [11].
Conclusion
PCR is a recent technique with a specificity ranging from 92% to 98% allowing early diagnosis. However, since histopathological diagnosis was made without a need for this method, we did not apply the PCR method. In conclusion, possibility of tuberculous etiology should be kept in mind in any patient with unexplained arthritis of the SC joint in an endemic region and susceptible population. A high index of suspicion is mandatory for timely diagnosis and treatment and non-responders to ATT must be looked for drug resistance or an immunocompromised state.
Conflict of Interest
The authors whose names are listed immediately below certify that they have no affiliations with or involvement in any organization or entity with any financial interest in the subject matter or materials discussed in this manuscript.
REFERENCES
- Tuli S.M.: Tuberculosis of the skeletal system: bones, joints, spine and bursal sheaths. Indian J Orthop. 2010;44:356.
- Lee S.H., Abramson S.B.: Infections of the musculoskeletal system by M. Tuberculosis. In: Rom WN, Garay SM (editors) Tuberculosis. 1996;635-644.
- Yasuda T., Tamura K., Fujiwara M.: Tuberculous arthritis of the sternoclavicular joint. A report of three cases. J Bone Joint Surg Am. 1995;77:136-139.
- Shah J.: Tuberculosis of sternum and clavicle: imaging findings in 15 patients. Skeletal Radiol. 2000;29:447-453.
- Dhillon M.S. Gupta R.K., Bahadur R., et al.: Tuberculosis of the sternoclavicular joints. Acta Orthop Scand. 2001;72:514-517.
- Martini M.: Tuberculosis of the bones and joints . 1988:149-150.
- Kurtz B., Hauss P.A., Druesne L., et al.: Tuberculosis arthritis of the sternoclavicular joint. Rev Med Interne. 2005;26:251-253.
- Singh S., Nagaraj C., Khare G.N., et al.: Multicentric tuberculosis at two rare sites in an immunocompetent adult. J Orthop Trauma. 2011;12:223-225.
- Shrivastav A., Pal P.S., Karmakar et al.: Tuberculosis of sternoclavicular joint-uncommon manifestation of a common disease. J Med. 2010;11:102-104.
- Blaustein S., Wysell M.: Pulmonary and skeletal tuberculosis. Mt Sinai J Med. 1997;64:419.
- Hazra A., Laha B.: Chemotherapy of osteoarticular tuberculosis. Indian J Pharmacol. 2005;37:5-12.



 Journal of Orthopaedics Trauma Surgery and Related Research a publication of Polish Society, is a peer-reviewed online journal with quaterly print on demand compilation of issues published.
Journal of Orthopaedics Trauma Surgery and Related Research a publication of Polish Society, is a peer-reviewed online journal with quaterly print on demand compilation of issues published.