Avascular necrosis of talus simulating juvenile idiopathic arthritis
Received: 27-Sep-2017 Accepted Date: Oct 23, 2017 ; Published: 25-Oct-2017
This open-access article is distributed under the terms of the Creative Commons Attribution Non-Commercial License (CC BY-NC) (http://creativecommons.org/licenses/by-nc/4.0/), which permits reuse, distribution and reproduction of the article, provided that the original work is properly cited and the reuse is restricted to noncommercial purposes. For commercial reuse, contact reprints@pulsus.com
Abstract
Avascular necrosis after fracture of the talus is well recognized, but is very rare in children. We report a case of avascular necrosis of the talus simulating juvenile idiopathic arthritis. The diagnosis was confirmed by open biopsy, and non-operative treatment was performed. The patient was asymptomatic with full range of motion postoperatively for two years. We hypothesize that avascular necrosis of the talus without fracture and dislocation might be caused by soft tissue damage around the talus with repeated hyperflexion of the ankle joint and slow arterial occlusion.
References
Blog | Yacht Charter in Greece Best Betting Sites in Indonesia Blog | Yacht Charter in Croatia Find Lawyer in Connecticut Blog | Yacht Charter in Italy Find Lawyer in Maryland Blog | Yacht Charter in Japan Info Blockchain Technologies Blog | Yacht Charter in Philippines Obgyn Journals Blog | Yacht Charter in Saudi Arabia Education Technologies Articles Blog | Yacht Charter in Turkey Cooling Technologies Articles Blog | Yacht Charter in UK Find Lawyer in New York Blog | Yacht Charter in USA Web Technologies Articles Blog | Places to Visit in Australia Best Betting Sites in VenezuelaKeywords
Talus, Juvenile, Avascular necrosis
Abbreviations
JIA: Juvenile Idiopathic Arthritis; Hb: Hemoglobin; WBC: White Blood Cell; CRP: C-Reactive Protein; ACPA: Anti-Cyclic Citrullinated Peptide Antibody; MRI: Magnetic Resonance Imaging; CT: Computed Tomography; ROM: Range Of Motion.
Level of Evidence: Level V
Introduction
It is sometimes difficult to differentiate juvenile idiopathic arthritis (JIA) from conditions such as infections, tumors, and reactive arthritis [1,2]. We encountered a case of avascular necrosis of the talus simulating juvenile idiopathic arthritis. Avascular necrosis of the talus after severe ankle injury is well recognized [3]. Fractures of the talus are extremely rare in children, and the reported incidence varies between 0.01 and 0.08% [4-6]. To the best of our knowledge, there have been no reports of avascular necrosis of the talus without fracture and dislocation in children. Here we report a case of avascular necrosis of the talus without fracture and dislocation.
Case Report
A two-year-old child developed swelling in his left ankle and limped while walking, and thus a physician was consulted. The physician could not detect the cause of his condition and referred him to us. His parents stated that he had swelling in his left ankle and was limping. He had no systemic symptoms and no remarkable medical or family history.
Regarding the physical examination, swelling, redness, localized heat, and effusion of the left ankle joint were observed. The range of his ankle motion was 10° dorsiflexion to 40° plantarflexion, and there were no signs of damage to ligaments. No swelling of the other joint was observed.
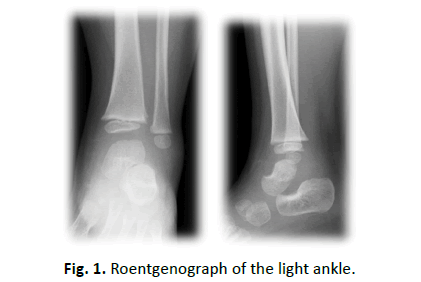
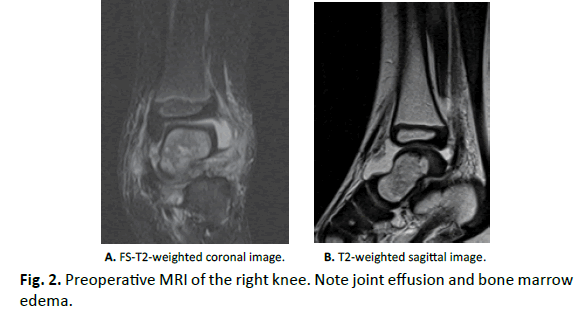
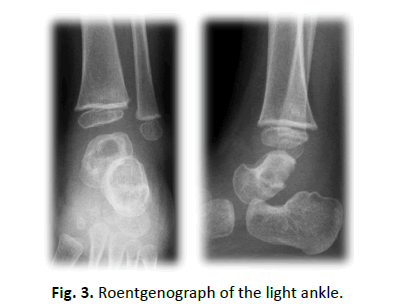
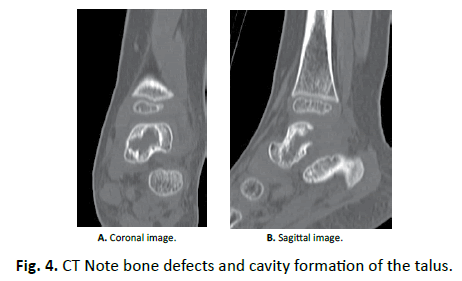
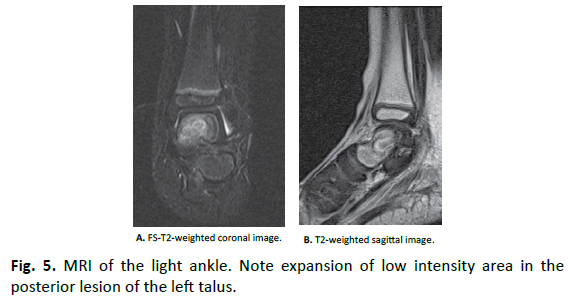
Laboratory tests revealed that Hb was 11.5 g/dl, WBC was 15300, and CRP was 1.17 mg/dl. Rheumatoid factor, anti-cyclic citrullinated peptide antibody (ACPA), and anti-nuclear antibodies were negative. Aspirated synovial fluid was bloody, and bacterial culture was negative. X-ray showed slight osteosclerosis of the talus of the left ankle (Fig. 1). MRI showed joint effusion and an edematous area in the bone marrow of the left talus, with no obvious abnormalities of articular cartilage (Fig. 2). One week after aspiration of joint fluid, CRP was 0.04 mg/dl, and no symptoms were found. However, X-ray showed bone defects and cavity formation in the talus of the left ankle three weeks later (Fig. 3). CT also demonstrated bone defects and cavity formation in the talus (Fig. 4). MRI showed expansion of a low intensity area in the posterior lesion of the left talus (Fig. 5).
An incision of approximately 2.5 cm was made and the talus was identified by an anterior approach. Macroscopically, articular cartilage was intact, and slight synovial hypercellularity was noted. Open biopsy was performed to obtain a partial bone sample from the disease foci. The bone defect site was filled with artificial bone graft.
Histological examination revealed osteonecrosis and mild chronic non-specific synovitis, including proliferation of lymphocytes and the presence of granulation tissue. These findings were highly suggestive of idiopathic or posttraumatic avascular necrosis. We then discussed the patient’s medical history with his parents again. They informed us that they recalled that his ankle joint may have once been hyperplantarflexed continuously by sliding over grass in a sleigh, but that he had no symptoms one month after the accident. From this medical history, we diagnosed this case to be posttraumatic avascular necrosis of the talus.
After open biopsy, ankle-foot orthosis was applied to the right leg for two months. ROM exercise and partial weight-bearing were started with a lower leg brace.
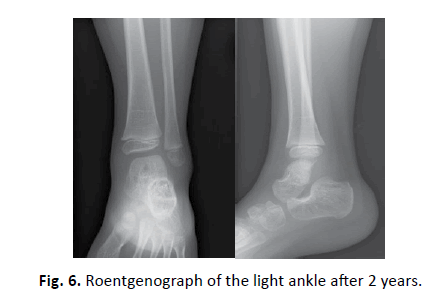
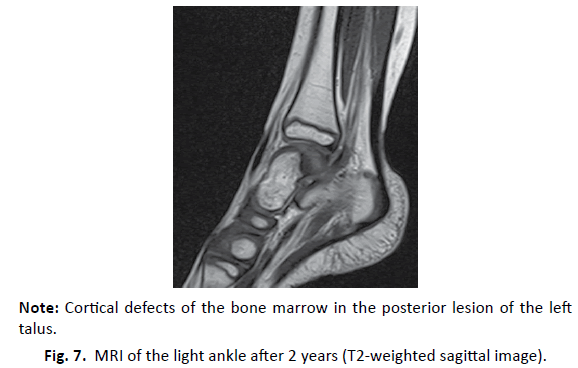
Two years after open biopsy, X-ray showed the disappearance of osteosclerosis and remodeling of the posterior portion of the talus (Fig. 6). MRI showed cortical defects of the bone marrow in the posterior lesion of the left talus, with no obvious abnormalities of articular cartilage (Fig. 7).
The patient was asymptomatic with full range of motion postoperatively for two years.
Discussion
Possible diseases that initially needed to be considered in this patient were JIA, infection, neoplasms, reactive arthritis, and hemophilia. At first, we examined a diagnosis of JIA or infection. Except for the left ankle, the patient had no other joint symptoms. The laboratory findings were equivocal to JIA or infection. From the histological findings of open biopsy, a diagnosis of avascular necrosis of the talus was made. Avascular necrosis after fracture of the talus is well recognized. Hawkins reported that the characteristic blood supply of the talus makes it prone to avascular necrosis, especially in fractures of the talar neck [7-10]. Rammeit [10] reported that fracture of the talus is very rare in juveniles, and long-term or multicenter clinical studies have only reported between one and two dozen cases [8].
At first, we considered a diagnosis of atraumatic osteonecrosis because there was no traumatic medical history. Pathogenesis of atraumatic osteonecrosis has been reported in association with several conditions, such as hyperlipidemia, hyperuricemia, occlusive vascular disease, systemic lupus erythematosus, sicklecell disease, alcoholism, and pancreatitis, as well as with the use of corticosteroids [9-11]. After detailed descriptions of the patient’s past history were obtained after open biopsy, a diagnosis of posttraumatic avascular necrosis of the talus was made. However, this patient had no symptoms one month after the accident. According to Mulfinger, avascular necrosis of the body of the talus after a simple fracture of the neck indicates unrecognized soft tissue damage around the talus with arterial occlusion from soft tissue swelling or arterial rupture from dislocation [12]. As for the pathogenic mechanism, avascular necrosis of the talus without fracture and dislocation might be caused by soft tissue damage around the talus with repeated hyperflexion of the ankle joint and slow arterial occlusion. The posterolateral corner of the talus, which receives the lowest blood supply, was osteonecrotic.
Non-operative treatment, core decompression, or arthrodesis can be considered for the treatment of avascular necrosis of the talus. In this patient, non-operative treatment was selected because the patient was young and did not remain symptomatic. The most effective period for partial weight-bearing and use of ankle-foot orthosis is controversial. There have been no controlled studies comparing early functional treatment with gradual weight-bearing and prolonged non-weight-bearing. Rammeit reported no clear advantage of prolonged non-weight-bearing and non-weightbearing only for the duration of the symptoms of pain and swelling is recommended [10]. In this case, the non-weight-bearing period was two months. There is no clear disadvantage of non-weightbearing.
Conclusion
We reported a case of avascular necrosis of the talus without fracture simulating juvenile idiopathic arthritis. The diagnosis was confirmed by open biopsy. We hypothesize that avascular necrosis of the talus without fracture and dislocation might be caused by soft tissue damage around the talus with repeated hyperflexion of the ankle joint and slow arterial occlusion.
REFERENCES
- Adleberg J.S., Smith G.H.: Corticosteroid-induced avascular necrosis of the talus. J Foot Surg. 1991;30:66-69.
- Cruess R.I.: Steroid-induced osteonecrosis: A review. Canadian J Surg. 1981;24:567-571.
- Draijer F., Havemann D., Beilstein D.: Verietzungs analyse kindlicher Talusfrakturen. Unfallchirug. 1995;98:130-132.
- Harris R.D., Silver R.A.: Atraumatic aseptic necrosis of the talus. Radiology. 1973;106:81-83.
- Hawkins LG. Fractures of the neck of the talus. J Bone and Joint Surg. 1970;52-A:991-1002.
- Jensen I., Wester J.U., Rassmussen F., et al.: Prognosis of fracture of the talus in children. A 21-year follow-up of 14 cases. Acta Orthop Scand. 1994;65:398-400.
- Lancaster S., Horowitz M., Alonso J.: Subtalar dislocations: a prognosticating classification. Orthopedics. 1985;8:1234-1240.
- Mulfinger G.L., Trueta J.: The blood supply of the talus. J Bone and Joint Surg. 1970;52-A:160-167.
- Prakken B., Albani S., Martini A.: Juvenile idiopathic arthritis. Lancet. 2011;377:2138-2149.
- Rammelt S., Zwipp H., Gavlik J.M.: Avascular necrosis after minimally displaced talus fracture in a child. Foot Ankle Int. 2000;21:1030-1036.
- Ravelli A., Martini A.: Juvenile idiopathic arthritis. Lancet. 2007;369:768-778.
- Schmidt M., Havemann D., Behrens P.: Talusfrakturen bei Kinderm und Jugendlichen. In: Rahmanzadeh R, Breyer HG. (eds.):Vertetzungen der unteren Extremitaten bei Kindem und Jugendlichen. Springer- Verlag, Berlin,1990; p. 337-339.



 Journal of Orthopaedics Trauma Surgery and Related Research a publication of Polish Society, is a peer-reviewed online journal with quaterly print on demand compilation of issues published.
Journal of Orthopaedics Trauma Surgery and Related Research a publication of Polish Society, is a peer-reviewed online journal with quaterly print on demand compilation of issues published.