Case report: Ulnar Nerve Leprosy Abscess-Palsy (UNLAP) diagnosis and treatment
Received: 10-Aug-2018 Accepted Date: Sep 25, 2018 ; Published: 02-Oct-2018
This open-access article is distributed under the terms of the Creative Commons Attribution Non-Commercial License (CC BY-NC) (http://creativecommons.org/licenses/by-nc/4.0/), which permits reuse, distribution and reproduction of the article, provided that the original work is properly cited and the reuse is restricted to noncommercial purposes. For commercial reuse, contact reprints@pulsus.com
Abstract
Pure Ulnar Nerve Leprosy Abscess-Palsy (UNLAP) is uncommon infectious disorder caused by Mycobacterium leprae. This study demonstrates a case report of isolated tubercloid leporsy neuritis of right ulnar nerve presented by sudden onset non-inflammatory tender oval swelling over elbow joint and complicated by acute motor and sensory deficit, posing a diagnositic management confusion. High resolution ultrasonography and maganatic resonance imaging (contrast and non-contrast) were performed. Swelling was expolred and excised after abscess evacuation with complete external neurolysis of ulnar nerve in the cubital tunnel. Specimen was taken for histopathological investigation which revealed positive special staining for leprosy. A typical presentation of leporsy must be taken into consideration to detect the proper line of treatment.
Keywords
Leprosy, ulnar nerve abscess, tuberculoid, hyperintense
Introduction
Leprosy (Hansan’s disease) is a non-fatal, slowly progressive chronic granulomatous infection which was first described by ancient Indians from sixth century B.C.1. [1] There is preferential involvement of the skin, peripheral nervous system, eyes, upper respiratory tract and testes because of their lower temperature than the core body temperature. [2] The neurophilic property of Mycobacterium leprae and immunity response reactions results in much debilitation and disfiguration and consequent psychosocial affection.
According to immunity state of exposed human, leprosy may extend from polar tuberculoid to polar lepromatous leprosy [3]. Patients with Borderline Tuberculoid (BT) form may be at high risk of nerve abscess, most commonly the ulnar nerve [4]. This article illustrates a case report of pure isolated ulnar nerve tubercloid leprosy abscess complicated by acute motor and sensory deficit, preoperative investigations done for possible diagnosis and the line of treatment performed.
Case Reports
A 25-year-old male presented with sudden onset throbbing pain and tingling\numbness sensation along the inner aspect of his right lower arm, medial aspect of right forearm, the hypothenar eminence of his hand and medial half of ring finger\whole little finger for twenty one day’s duration. There was no history of fever. Superficial thick cordlike swelling was palpated behind medial epicondyle and supracondylar ridge.
Physical examination revealed tender thickened right ulnar nerve for approximately 9.0 cm proximal and 6 cm distal to the medial epicondyle of the humerus respectively. Multiple soft nodules were palpable along the course of the nerve. Complete clawing was noticed with inability to extend the interphalangeal joints of the middle and ring finger. No wasting of thenar, hypothenar and 1st dorsal interossi muscle. Sensation was diminished for along medial aspect of right forearm, hypothenar eminence and medial half of ring finger\whole little finger. There were no local trophic changes. The rest of the physical examination including the eyes, testes and nose did not reveal any abnormality.
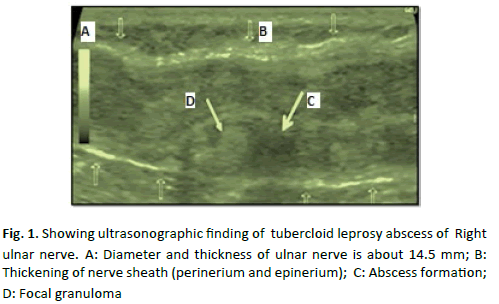
Skins smear is negative for acid fast bacilli. High resolution ultrasonography revealed nodular thickening of the right ulnar nerve proximal and distal to the medial epicondyle for a length of approximately 9.0 cm and 6 cm respectively. The maximum diameter of the nerve was 14.5 mm. Swollen heterogeneous hypoechoic nerve fascicles with echogenic perineurium and epineurium was revealed. Multiple focal outpouchings lesions were also noted arising from the nerve (Fig. 1).
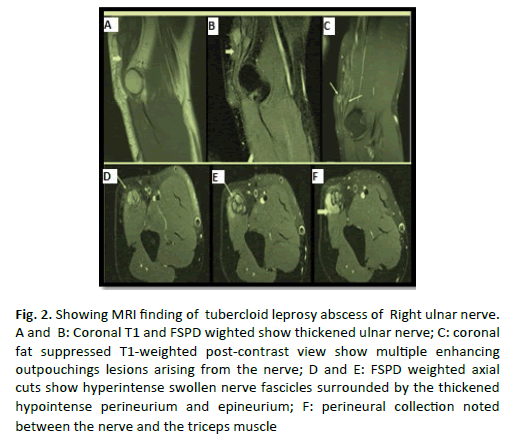
MRI (Non-contrast and contrast-enhanced) finding revealed nodular thickened right ulnar nerve for an approximate length of 9.0 cm proximal and 6.0 cm distal to the medial epicondyle. The maximum thickness of the nerve was 14.5 mm. Swollen nerve fascicles appeared mildly hyperintense signal to muscle on T1-weighted images and markedly hyperintenseon Fat-Saturated Proton Density (FSPD) and Thickened hypointense perineurium and epineurium appeared on all sequences with its multiple disruptions by small contiguous variable sized outpouchings. A ‘horse-shoe’ shaped noted between the nerve and the triceps muscle and epineural collection (mildly hyperintense to muscle on T1-weighted images and strongly hyperintense on FSPD and T2-weighted images) are characteristic of abscess collection around nerve sheath. Post-contrast images revealed multiple focal outpouching enhancements of the nerve and neural sheath (Fig. 2).
Figure 2: Showing MRI finding of tubercloid leprosy abscess of Right ulnar nerve. A and B: Coronal T1 and FSPD wighted show thickened ulnar nerve; C: coronal fat suppressed T1-weighted post-contrast view show multiple enhancing outpouchings lesions arising from the nerve; D and E: FSPD weighted axial cuts show hyperintense swollen nerve fascicles surrounded by the thickened hypointense perineurium and epineurium; F: perineural collection noted between the nerve and the triceps muscle
Based on physical examination and preoperative imaging studies, a provisional diagnosis of isolated ulnar neuritis with abscesses was considered.
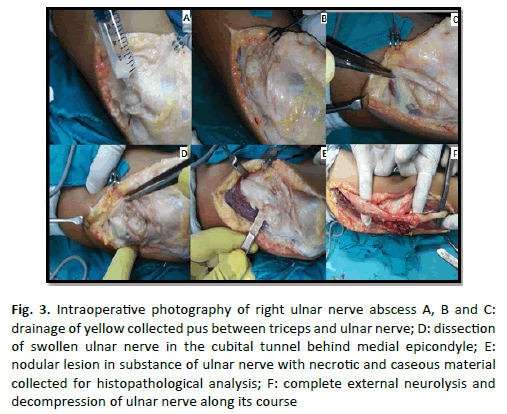
The patient was operated for ulnar nerve decompression and abscess evacuation using standard posterior approach of elbow joint in lateral decubitus position ; identification of ulnar nerve course in the cubital tunnel; yellow pus evacuation and collection for culture and sensitivity; external ulnar nerve neurolysis along its course extending proximally above medial epicondyle from ulnar nerve piercing medial intermuscular septum at ligament of struthes to distally below medial epicondyle at entrance of ulnar nerve between 2 heads of flexor carpi ulnaris; specimens from nerve, its sheath and outpouching lesions were collected for histopathological analysis to confirm diagnosis and detection of causative microorganisms (Fig. 3).
Figure 3: Intraoperative photography of right ulnar nerve abscess A, B and C:drainage of yellow collected pus between triceps and ulnar nerve; D: dissection of swollen ulnar nerve in the cubital tunnel behind medial epicondyle; E:nodular lesion in substance of ulnar nerve with necrotic and caseous material collected for histopathological analysis; F: complete external neurolysis and decompression of ulnar nerve along its course
Postoperatively, the patient was assumed to have recurred by early restoration of hand functions, recovery of hand clawing and preservation of sensation along dermatological distribution of ulnar nerve. Histopathological specimens revealed extensive caseation material with Langerhans-epithloid cell granuloma along nerve’s course and modified Ziehl-Nelsen staining revealed acid fast bacilli suggestive of Mycobacterium leprae. After confirmation of tuberculoid ulnar nerve leprosy lesion, the patient was put on a course of anti-inflammatory drugs, steroids and Anti-Leprosy Therapy (ALT) (Dabasone) besides neurotonic therapy to enhance nerve recovery. On follow-up after one and half month, the patient was completely relieved with significant reduction in the ulnar nerve thickening without any sensorimotor deficit.
Discussion
Leprosy neuritis without dermatolgical involvement is characterized by nerve enlargment, nerve pain, somatosensory dysfunction and muscle wasting and this poses a difficulty in diagnosis especially in absence of nerve biopsy [5]. Japling 1965 was the 1st who reported pure leportic neuritis with negative skin leprotic mainfestation and described cold abscess of peripheral nerve [6]. The incidence of leprosy nerve abscesses has been increasing. Young children and teenagers account for the majority of cases [7]. Ulnar nerve is the commonest nerve to form tuberculoid leprosy abscesses [8]. Approximately 1.3% of leprosy patients form a nerve abscess and some of them may calcify as recorded in Indian population [9]. Leprosy neural involvement is obviously observed across the disease entity and in lepra reactions. Particularly in BT leprosy, usually granuloma is the commonest neural lesion but unusual an abscess formation [10]. Aggressive epithelioid and lymphoid cells infiltration into the nerve is hallmark pathology in tuberculoid leprosy causing epineurium\perineurium thickening, extensive nerve enlargement and destruction of fascicles. However, preservation of the neural architecture is better in lepromatous than tuberculoid lesion due to mild immune response and active proliferation of bacilli occurs. Tissue hypoxia and pressure from inflamed swollen neuronal fascicles leads to avascular necrosis and abscess formation [11,12] .
The demonstrated case was mainfested by acute painful nodular swelling behind medial epicondyle along the course of Right ulnar nerve with motor and sensory deficit without any lepromatous dermatological mainfestation and negative skin smear for acidfast bacilli. Noninvasive preoperative investigation (ultrasonography and MRI) revealed thichened enlarged ulnar nerve with fluid most probably pus collecting between nerve sheath and adjacent tricipes muscle and also muliple nodular lesion along its course. All of clinical and radiogical finding are suggestive for surgical expolartion of ulnar nerve aiming for pus drainge,debridement, external neurolysis and decompression of ulnar nerve.
Histopatholgical analysis of collected specimen (pus and caseous material from nodular lesion) is the only tool to confirm tubercloid leporsy due to occasional inability to determine Mycobacterium bacilli by fine needle aspiration biopsy as leprosy is of pauci bacillary spectrum of disease [13].
Conclusion
In conclusion, awerness of a typical mainfestation of leporsy like leportic neuropathy must be taken into account and without complacency. Surgical debridement, specimen collection and nerve decompression is manadatory in this case to detect causative organism; also to avoid more motor\sensory deterioration and complications if left untreated like rupture and sinus formation resulting in 2ry bacterial infection and chronicity [14].
REFERENCES
- Gelber R.H.: Harrison's principles of internal medicine 18th ed. New York: McGraw Hill. 2012:1359-1366.
- McAdam A.J., Sharpe A.H.: Robbins and cotran pathologic basis of disease 8th ed. philadelphia: saunders elsevier; 2010:372-374.
- Job C.K., Desikan K.V.: Pathological changes and their distrubation in peripheral nerves in leporamatous leporsy. Int J Lepra Other Mycobact Dis.1968;36:257-270.
- Kumer P., Saxena R., Mahan L., et al.: Peripheral nerve abscess in leporsy: report of twenty cases. Idian J Lepr 1997;69:143-147.
- Jenkins D., Papp K., Jakubovic H.R., et al.: Leprotic involvement in peripheral nerves in the absence of skin lesions. J Am Acad Dermatol.1990;23:1023-1026.
- Japling WH.: Pure neural tubercloid leporsy. Britan Med J 1965;2:799-800.
- Salafia A., Chauhan G.: Nerve abscess in children and adult leprosy patients: analysis of 145 cases and review of the literature. Acta Leprol. 1996;10:45–50.
- Hari S., Subramanian S., Sharma R.: Magnetic resonance imaging of ulnar nerve abscess in leprosy: A case report. Lepr Rev. 2007;78:155-159.
- Lichtman D.M., Swafford A.W., Kerr D.M.: Calcified abscess in the ulnar nerve in a patient with leprosy. J Bone Joint Surg.1979;61:620-621.
- Kulkarni M., Chauhan V., Bharucha M., et al.: MRI imaging of ulnar leprosy abscess. JAPI. 2009;57:175-176.
- Thomas M., Emmanuel M.: Facial nerve abscess in a case of leprosy-a case report. Neurol Asia. 2009;14:41-42.
- Bianchi S., Martinoli C.: In: Ultrasound of the musculoskeletal system. Baert A.L., Knauth M., Sartor K..: Medical radiology: diagnostic imaging and radiation oncology. Berlin Heidelberg: Springer-Verlag. 2007:112–114.
- Vijaykumar M., D'Souza M., Kumar S., et al.: Fine needle aspiration cytology (fnac) of nerves in leporsy. Lepr Rev 2001;72:171-178.
- Saxena U., Ramesh V., Misra R.S.: Gaint nerve abscess in leporsy. Clin Exp Dermatol. 1990;15:349-351.



 Journal of Orthopaedics Trauma Surgery and Related Research a publication of Polish Society, is a peer-reviewed online journal with quaterly print on demand compilation of issues published.
Journal of Orthopaedics Trauma Surgery and Related Research a publication of Polish Society, is a peer-reviewed online journal with quaterly print on demand compilation of issues published.