Comminuted fracture of the trapezium associated with trapeziometacar-pal joint dislocation: A report of a rare case and a review of literature
Received: 13-Aug-2020 Accepted Date: Sep 18, 2020 ; Published: 28-Sep-2020
This open-access article is distributed under the terms of the Creative Commons Attribution Non-Commercial License (CC BY-NC) (http://creativecommons.org/licenses/by-nc/4.0/), which permits reuse, distribution and reproduction of the article, provided that the original work is properly cited and the reuse is restricted to noncommercial purposes. For commercial reuse, contact reprints@pulsus.com
Abstract
In this paper we report and discuss the management of an extremely rare case of comminuted trapezium fractures associated with Trapeziometacarpal (TMC) joint dislocation. To our knowledge only 2 cases were reported in the literature. Treating such injury is challenging. The aim when treating such fractures is to maintain fracture stability preventing further displacement while maintaining reasonable joint congruity. Although short-term outcomes are satisfactory, it is hard to predict long-term complications.
Keywords
Trapezium fracture, trapezium treatment, carpal fracture, trapeziometacarpal joint dislocation
Introduction
Trapezium fractures are rare, accounting for less than 5% of all carpal bone fractures. Less commonly it is associated with Trapeziometacarpal (TMC) joint dislocation. Most reported cases of trapezium fracture with TMC dislocation are vertical oriented fractures (walker type II a and Type IV). To our knowledge only two authors reported TMC joint dislocation with comminuted trapezium fracture [1,2]. Each treated this injury differently. In this article, we wish to share our experience with this unusual injury.
Case Presentation
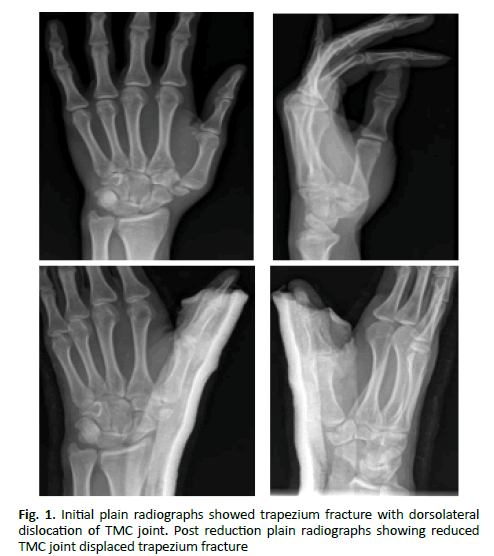
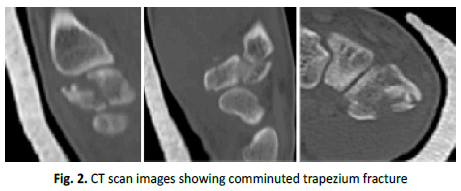
Our patient is a 30 years old military personnel presented to the emergency department after he fell from a motor bike. He came complaining of pain and inability to move his left thumb. Clinical examination showed left thumb shortening with obvious dorsal-radial swelling at the thumb base. There was tenderness at the base of the thumb with no tenderness at the snuffbox. Thumb range of motion was limited due to pain and distal neurovascular was intact. Initial plain radiographs showed, trapezium fracture with dorsal and radial displaced TMC joint dislocation. In the emergency department reduction was performed with axial thumb traction and by applying simultaneous pressure over the lateral aspect of the thumb base. A pulpable click was felt and thumb spica-slab was applied. Reduction was confirmed with plain imaging. CT was then performed and showed a displaced and comminuted trapezium fracture. There were no associated metacarpal or other carpal fractures.
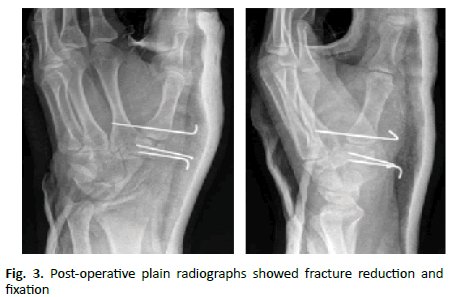
The patient was admitted for operative intervention. In the operating room, closed reduction was performed under image guidance and two parallel k-wires were placed throw the trapezium to maintain reduction one k-wire was then placed from the first to second metacarpal bone to unload the joint (Fig. 1). Reduction and stability were satisfactory intraoperative. Thumb-spica slab was added for additional stability and to alleviate the pain (Fig. 2). Thumb-spica slab and k-wires were removed after 6 weeks and physiotherapy started (Fig. 3).
Results
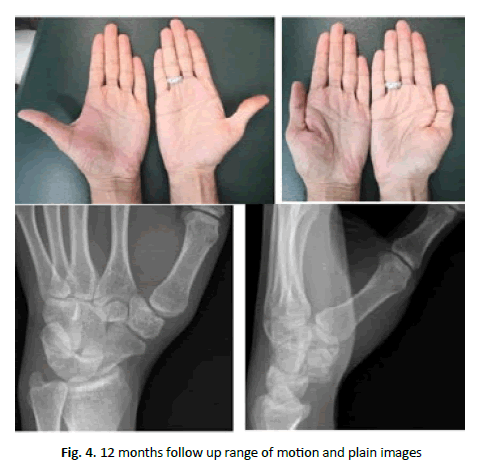
At 12 months follow up, his range of motion was equal to the unaffected side. His grip strength was measured with a Jamar dynamometer and was 55 Kg while the right side (normal side) was 80 Kg. The thumb function score was 10/10 on the Kapandji scale. The patient did not complain or show any signs of TMC instability. His VAS pain score was 4/10 when lifting heavy objects. He reported on and pain at rest but it did not affect his level of activity. The patient was able to return to his job and resume his military duties. X-rays showed complete healing of the fracture and a congruent TMC joint (Fig. 4).
Discussion
The trapezium is the most radial carpal bone found in the distal carpal row. It articulates proximally with the scaphoid and trapezoid and distally with the first metacarpal. It has a unique double saddle articulation with the base of the first metacarpal which gives the thumb its unique multiplanar movement. It is important to preserve the joint congruity to maintain its vast range of motion [3].
TMC joint is very stable construct. Its stability is well maintained by the function of 16 ligaments. Biomechanical studies have shown that joint reactive forces at thumb TMC joint are 12 times greater than that generated at the tip of the thumb with lateral pinch, and compressive forces of as much as 120 kg may occur at the TMC joint with forceful grasp. Integrity of the joint’s stability is important to have an effective pinch and grip [4,5].
Isolated TMC joint dislocation is extremely rare, accounting less than 1% of hand injuries. Failure of this stable construct requires a large force and majority are throw trans-osseous fractures [6,7].
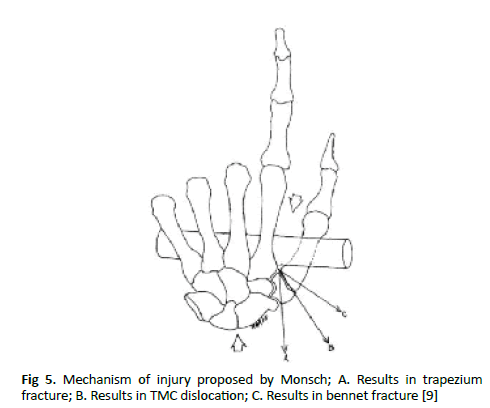
There are two proposed mechanisms of trapezium fracture and TMC joint dislocation [8,9]. The direct mechanism by Monsch, were the force is directed through the first web space. This could occur when an object is fixed at the first web space (example: holding the handle of a motor bike) while falling, forcing the hand against the object. This causes a commissural sheering force through the thumb base. The structures injured are related to the magnitude and direction of force during trauma (Fig. 5). The indirect mechanism is an axial force in a flexed first metacarpal. This leads to impaction of metacarpal base on the body of the trapezium. Forces travel indirectly from the first metacarpal to the TMC joint and the trapezium. Depending on the position of the first metacarpal and wrist the type of trapezium fracture will occur.
Figure 5: Mechanism of injury proposed by Monsch; A. Results in trapezium fracture; B. Results in TMC dislocation; C. Results in bennet fracture [9]
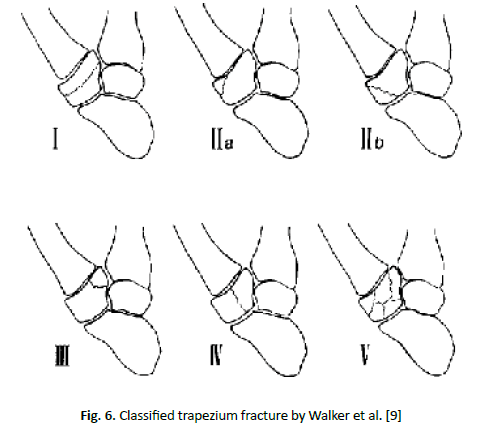
Walker et al. classified trapezium fracture into 5 types based on fracture morphology [9]. Type I is a horizontal extra-articular fracture. Type IIa and IIb are vertical fractures of the radial tuberosity involving both the TMC and scaphotrapezial joint respectively. Type III is a vertical ulnar tuberosity fracture through the TMC joint. Type IV and V involves both TMC and scaphotrapezial joints but type IV is vertical and V is comminuted. According to the literature, most trapezium fracture associated with TMC joint dislocation are type IIa and type IV fractures and less often type V. This is because of loss of structural support at the thumb base making the joint unstable allowing the metacarpal bone to slide dorsal and radial.
Early identification and management of such fractures are significant to preserve thumb motion and function [10]. Authors reported missed trapezium fracture that led to less desirable outcome. Samson et al. reported non-union of the trapezium due to missed fracture. The patient eventually regained his function and was pain free after delayed operative treatment [10] (Fig. 5).
Treatment varied between authors. It ranged from closed reduction and casting, closed reduction and k- wiring, open reduction and internal fixation to arthroscopic assisted internal fixation [1,7,11,12]. Authors decision for operative intervention was based on post reduction stability and amount of fracture displacement. We believe that vertical oriented fractures and fractures associated with TMC joint dislocation are unstable fractures and are better stabilized [10].
Treatment of comminuted trapezium fractures is challenging. Highly comminuted fracture pattern like our case is not amenable for internal fixation. Most authors agreed to treating such fractures by traction or distraction. Internal fixation might lead to more comminution and achieving adequate stability is difficult. We aimed to achieve reasonable reduction and maintain adequate stability, preventing further displacement or dislocation while, restore original height and maintaining a reasonable joint congruity.
Regardless of mode of treatment and type of fracture almost all reported good short-term outcomes [13]. Unfortunately, long term follow-up is lacking. Only few follow their patients for longer than 2 years. McGuigan et al. followed up 11 patients with trapezium fracture who underwent operative treatment for an average of 48 month [14]. 8 reported some pain in the TMC joint but did not affect their function. Almost half of the patients showed degenerative changes on plain radiographs. Kohayama et al. [2] performed an open reduction and elevation of articular surface was with tricalcium phosphate [13]. Initially the patient returned his pre-injury function. At 2 years follow up although the patient had pain free full range of motion, a zigzag deformity was noticed on x-ray with hyperextension. Which is usually seen with TMC joint osteoarthritis. He concluded that this might be due to unrecognized ligament injury that led to some joint instability and latter degeneration (Fig. 6).
Figure 6: Classified trapezium fracture by Walker et al. [9]
Few reported residual TMC joint instability after the fracture has healed. Kohyama et al. [2] thinks that the late radiological joint degeneration is related to missed ligamentous injury that was not addressed. Therefore, longer follow up might be needed to assess residual instability.
Conclusion
Comminuted fracture of the trapezium with TMC joint dislocation is extremely rare. Early identification and management of such fractures are significant to preserve thumb motion and function. Post reduction assessment of stability is mandatory. The aim when treating such fractures is to maintain fracture stability and prevent further displacement while maintaining reasonable joint congruity. Longer follow up is advisable to assess joint function and residual instability. Although short-term outcomes are satisfactory, it is hard to predict long-term complications.
REFERENCES
- Alonso L., Couceiro J.: Comminuted fracture of the body of the trapezium and thumb carpometacarpal dislocation: a particular pattern. J Surg. 2018;4:34-36.
- Kohyama S., Tanaka T., Ikumi A., et al.: Trapezium fracture associated with thumb carpometacarpal joint dislocation: a report of three cases and literature review. Case Rep Orthop. 2018;21.
- Su F.C., Lin C.J., Wang C.K., et al.: In vivo analysis of trapeziometacarpal joint anthrokinematics during multidirectional thumb motions. Clin Biomech. 2014;29:1009-1015.
- Roger J., Mathieu L., Mottier F., et al.: Trapeziometacarpal joint dislocateion complicated by a trapezium fracture: a case report and literature review. Hand Surg Rehab. 2016;35:288-291.
- Bettinger P.C., Linscheid R.L., Berger R.A., et al.: An anatomic study of the stabilizing ligaments of the trapezium and trapeziometacarpal joint. J Hand Surg. 1999;24:786-798.
- Garneti N., Tuson C.E.: Sagittally split fracture of trapezium associated with subluxed carpo-metacarpal joint of thumb. Injury. 2004;35:1172-1175.
- Parker W.L., Czerwinski M., Lee C.: First carpalmetacarpal joint dislocation and trapezial fracture treated with external fixation in an adolescent. Ann Plast Surg. 2008;61:506-510.
- Wiesler E., Chloros G., and Kuzma G.: Arthroscopy in the treatment of fracture of the trapezium. J Arth Rel Surg. 2007;23:1248-1248.
- Walker J.L., Greene T.L., Lunseth P.A.: Fractures of the body of the trapezium. J Ortho Trauma. 1988;2:22-28.
- Samson D., Jones M., Mahon A.: Non-union of the trapezium: rare consequence of a rare injury. J Surg Case Rep. 2018;4:1-3.
- Ramoutar D.N., Katevu C., Titchener A.G., et al.: Trapezium fracture-a common technique to fix a rare injury: a case report. Case J. 2009;2:8304.
- Garavaglia G., Bianchi S., Santa D.D., et al.: Transtrapezium carpo-metacarpal dislocation of the thumb. Arch Orthop Trauma Surg. 2004;124:67-68.
- Kose O., Keskinbora M., Guler F.: Carpometacarpal dislocation of the thumb associated with fracture of the trapezium. J Orthop Trauma. 2015;16:161-165.
- McGuigan F.X., Culp R.W.: Surgical treatment of intraarticular fractures of the trapezium. J Hand Surg. 2002;27:697-703.



 Journal of Orthopaedics Trauma Surgery and Related Research a publication of Polish Society, is a peer-reviewed online journal with quaterly print on demand compilation of issues published.
Journal of Orthopaedics Trauma Surgery and Related Research a publication of Polish Society, is a peer-reviewed online journal with quaterly print on demand compilation of issues published.