Comparative study of CT guided patient specific jig assisted TKA and conventional instrumentation TKA
Received: 14-Jul-2017 Accepted Date: Sep 22, 2017 ; Published: 25-Sep-2017
This open-access article is distributed under the terms of the Creative Commons Attribution Non-Commercial License (CC BY-NC) (http://creativecommons.org/licenses/by-nc/4.0/), which permits reuse, distribution and reproduction of the article, provided that the original work is properly cited and the reuse is restricted to noncommercial purposes. For commercial reuse, contact reprints@pulsus.com
Abstract
Purpose: Comparing the technology of CT guided jigs assisted surgery with conventional instrumentation system in restoring the mechanical axis in total knee arthroplasty.
Method: Randomized two groups of 10 patients each were operated by Conventional instrumentation and CT guided pre-designed patient specific jigs. Intra and postoperative blood loss, operative time and correction of mechanical axis was recorded and compared.
Results: Mean rotational femoral angle was 1.0° for cases group and 1.5° for the control group, difference was statistically significant. The difference in preoperative and postoperative HKA angles between case and control groups was found to be significant in both groups but more in cases group. The alignment of knee in cases was closer to ideal 6-degree valgus alignment than the control group. The mean PCV fall in postoperative period in case group was 2.66 and in control group was 3.5. The mean operative time using CT guided jigs was 52.80 min and that in control group using conventional instrumentation was 62.40 min.
Conclusion: Restoration of alignment axis and placement of femoral component was found to be more accurate with CT guided jigs as compared to conventional instrumentation. Patients having extra articular deformity in femur which hampers the insertion of alignment rod properly to assess the anatomical axis are benefited by these patient specific jigs which obviate the need for intramedullary rod insertion. PSI is more precise as compared to conventional system but tibial jig placement requires improvement as it’s less conforming than femoral jigs which can lead to intraoperative errors.
Keywords
TKA, Patient specific CT guided jig system, Conventional instrumentation
Abbreviations
CT: Computerized Tomography; MRI: Magnetic Resonance Imaging; TKR/A: Total Knee Replacement/Arthroplasty; PSI: Patient Specific Instrumentation; CI: Conventional Instrumentation; BMI: Body Mass Index; SPSS: Statistical Product and Service Solutions; FS-TS angle: Femoral Shaft and Tibial Shaft angle; HKA angle: Hip Knee Ankle angle; LDFA; Lateral Distal Femoral Angle; MPTA: Medial Proximal Tibial Angle; FM-FS angle: Femoral Mechanical axis: Femoral Shaft angle; CP angle: Condylar Plateau angle; VAS: Visual Analog Scale; KSS: Knee Society Score; PCV: Packed Cell Volume.
Introduction
Total knee arthroplasty is the treatment of choice for advanced arthritis of knee in patients with age above 50 years. It’s one of the advanced and evolving orthopedic surgeries. The aim of TKR is to achieve long-term successful functional outcome with minimal complications. Restoration of mechanical axes to the near normal is one of the prime predictors of successful outcome.
Component mal-positioning may lead to wear and loosening, ork patellar instability resulting in early failure and revision surgery [1,2]. As little as 3° of Varus/valgus angulations can significantly change the pressure distribution and total load in the medial and lateral compartments of the tibial component [3].
CI system is based on average bone geometry and relies on intramedullary rods and jig. Step that involves drilling hole in femur for intramedullary rod can lead to varus/valgus mal-alignment, notching and oversized component which have an implication on soft tissue balancing and life of the implant [4,5]. Conventional jigs consist of many components, assembling it can be time consuming and there is violation of intramedullary canal which can lead to post-operative bleeding, fat embolism and infection [6].
Computer assisted navigation system can improve alignment but increases operative time, expensive and it is still dependent upon the conventional instrumentation [7]. Initially MRI based jigs were introduced but due to cost considerations and time consumption, they were replaced by CT guided jigs.
Presently patient specific instrumentation is actually customized placement jigs for a specific patient using standard off-the-shelf knee implants. Either a CT or MRI is taken of the patient’s knee. The data is processed in a computer assisted design system, and the primary femoral and tibial placement jigs are designed and manufactured for that patient. Once the primary distal femoral cut and proximal tibial cut are completed, the remaining bone preparation is accomplished with standardized off the shelf instrumentation [8].
The aim of this study was to compare the technology of CT guided jigs assisted surgery with conventional instrumentation system in restoring the mechanical axis.
Materials and Methods
Patient Enrollment
It was a case series, with sample size of 20 patients randomized by computer scheme into 10 patients each for case group (PSI) and control group (CI) from January 2015 to March 2016. Sample size was dependent upon limited number of patients.
Patients with age >50 years and osteoarthritis (grade 3 and 4) who failed to improve on conservative management were included in the study. Exclusion criteria included Rheumatoid arthritis, large defects in tibia or femur requiring augmentation and previous knee infection or surgery.
Mean patient age was 62.5 years and Mean BMI was 32.3 kg/m2.
Informed Consent
Informed consent was taken from all patients.
Image Protocol
Radiographs and scanograms were obtained of the involved limb in both case and control groups. Non-contrast CT of the affected limb of case group involving from hip to ankle with 3 mm to 5 mm axial cuts and knee with 1mm axial cuts with field of vision 30 cm to 35 cm was performed at our institute. The data was sent to implant manufacturer who created 3D images and used Pre-plan 3-Matic software to design the jigs (Fig. 1). The preoperative plan included the amount of valgus and external rotation required in distal femoral cut and thickness of tibial cut for each individualized patient according to the various preoperative angles measured.
Operative Methodology
All operation followed by TKA surgical planning were conducted by an experienced surgeon. Both case and control groups were given injection tranexamic acid intraoperatively. Control group was operated using standard intramedullary anterior referencing instrumentation.
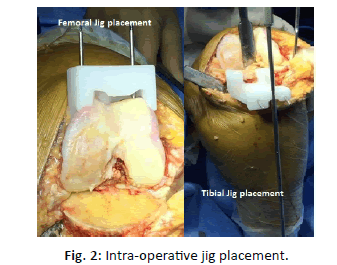
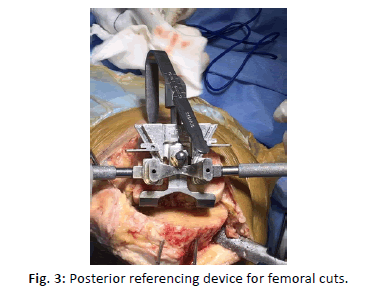
For case groups after the design approval by surgeon, it took 6 days to prepare the jigs. These patient specific jigs were only pinning guides, for distal femoral and proximal tibial cuts. The cutting jigs were placed at the site where the pins were already placed with the help of PSI jigs (Fig. 2). These jigs were used intraoperatively for the distal femoral cut and proximal tibial cut, the remaining bone preparation was accomplished with standardized off the shelf instrumentation. These jigs used the posterior referencing system for the distal femoral cut (Fig. 3).
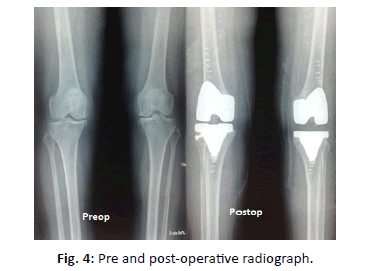
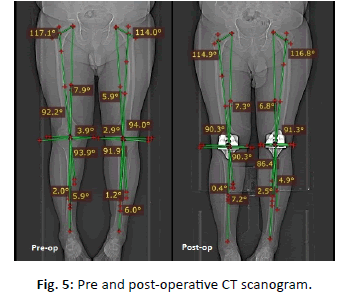
Implant size used, operative time, intra operative and post-operative (suction drain) blood loss was recorded. Post-operative radiographs (Fig. 4) and CT scanograms (Fig. 5) (within 3 months) were done to see mechanical alignment and rotational alignment of femoral and tibial implant.
Results
The data collected was analyzed using IBM SPSS v 22.0 software.
Goal of TKA surgery is to restore the normal alignment of the knee and various angles were compared. The mean FS-TS angle post operatively in cases group was 5.4 and in control was 2.5. Ideally there is 6-degree valgus alignment of knee. The alignment of knee in cases was closer to ideal 6-degree valgus alignment than the control group. The difference was statistically significant.
The mean HKA angle in postoperative patients was 183.5 (181 to 191) for conventional control group and 181.5 (180.4 to 182.2) for cases group. The difference in preoperative and postoperative HKA angles between case and control were found to be significant in both groups.
The mean rotational femoral angle was 1.0° (0.6° to 1.5°) for cases group and 1.5° (0.8° to 2.4°) for the control group. This difference was found to be significant.
There was no significant difference in LDF angle, MPT angle, HKA, FM-FS angle and CP angle. No significant difference in VAS score, KSS score, Knee range of motion and extensor lag.
The mean amount of hemoglobin fall in the postoperative period in case and control group was 0.95 g/dL and 1.35 g/dL respectively. While mean PCV fall in postoperative period in case and control group was 2.66 and 3.5 respectively. The mean drain output in case and control group was 110 mL (20 mL to 320 mL) and 212 ml (120 mL to 340 mL) respectively. The correlation of difference of hemoglobin in postoperative period in cases and control group was found to be insignificant but was significant for PCV fall and drain output.
The mean operative time using CT guided jigs was 52.80 min and that in control group using conventional instrumentation was 62.40 min, difference was statistically insignificant.
Discussion
One of the most important predictors of a successful TKA surgery depends on the restoration of the normal biomechanics of the knee. Mispositioning of the component can lead to failures due to aseptic loosening, instability, polyethylene wear and dislocation of the patella [1].
Study done by Sassoon [9] concluded that PSI for TKA has not reliably demonstrated improvement of postoperative limb or component alignment when compared with standard instrumentation.
Meta-analysis conducted by Thienpont [10] to examine the effect of PSI on radiological outcomes after TKA was done to assess the mechanical axis alignment and malalignment of the femoral and tibial components in the coronal, sagittal and axial planes, at a threshold of >3° from neutral. It concluded that PSI does not improve the accuracy of alignment of the components in TKA compared with CI.
As opposed to the meta-analysis, our study depicts, better alignment postoperatively in TKR patients using CT guided jig assisted TKR in terms of improved alignment of knee represented by HKA angle, FS-TS angle and femoral rotation as compared to conventional instrumentation.
PSI is particularly beneficial in certain cases like in knees with extra articular deformity in femur which hampers the insertion of alignment rod properly to assess the anatomical axis. This can lead to intraoperative error and faulty femoral cuts. PSI obviates the need for intramedullary rods. In our study, Case No. 1 and 2 had extra articular femoral bending which might lead to inappropriate alignment rod insertion, consequences of which can lead to faulty femoral cuts. The use of PSI obviates the need of intramedullary femoral rod insertion in these cases and thus preventing faulty femoral cuts and any fracture.
In our study the better alignment results with PSI on femoral side, may be due the fact the femoral jigs are better conforming to the anatomical contour of the femur whereas the tibial jigs need improvement in this aspect. The femoral jigs seat very well on the contour of the femur whereas tibial jig doesn‘t seat so well. Inadvertent removal of osteophytes and incomplete soft tissue stripping can lead to errors in tibial cuts.
One knee in PSI cases group suffered a fracture of lateral tibial condyle requiring fixation with cannulated screws which increased the operative time. As well as malalignment in the same case required multiple trial attempts of polyethylene insert and a rechecking alignment leading to increased operative time.
Boonen et al. [11] that demonstrated a 5-minute (P<0.01) reduction in operative time for PSI compared with off-the-shelf implants. According to the study conducted by Sassoon [9] there is decisive evidence exists to support that PSI requires fewer surgical trays, PSI has not clearly been shown to decrease the operative time.
In our study, the mean operative time using CT guided jigs was 52.80 minutes and that in control group using conventional instrumentation was 62.40 minutes. Though there is difference of 9.6 minutes but it wasn‘t found to be statistical significant.
Andrzej Kotela et al. [12] study concluded that the mean postoperative blood loss was 850 ± 450.5 mL in cases group and 1000 mL ± 502.1 mL in control group. In the postoperative period, blood transfusions were required in both groups. Our study showed similar result where PCV fall and drain output was less in case group.
Conclusion
1. Restoration of alignment axis and placement of femoral component was found to be more accurate with CT guided jigs as compared to conventional instrumentation.
2. PSI more beneficial in certain cases like in knees with extra articular deformity in femur where alignment rod insertion can lead to errors intraoperatively.
3. Femoral component of PSI jig is more conforming to bone contour than tibial component. Excessive removal of osteophytes and incomplete stripping of tissues can lead to errors in tibial component.
4. Post-operative blood loss and operative time is reduced in PSI as compared to CI.
5. We concluded that the CT guided PSI system is more accurate and precise than CI but further study is required to improve placement of tibial component.
REFERENCES
- Chang M.J., Lim H., Lee NR., et al.: Diagnosis, causes and treatments of instability following total knee arthroplasty. Knee Surg Relat Res. 2014;26(2):61-67.
- Jonsson B., Astrom J.: Alignment and long-term clinical results of a semi constrained knee prosthesis. Clin Orthop Relat Res. 1988;226:124-128.
- Werner F.W., Ayers D.C., Malestsky L.P., et al.: The effect of valgus/ varus malalignment on load distribution in total knee replacements. J Biomech. 2005;38:349-355.
- Stulberg S.D.: How accurate is current TKR instrumentation? Clin Orthop Relat Res. 2003;416:177-184.
- Delp S.L., Stulberg S.D., Davies B., et al.: Computer-assisted knee replacement. Clin Orthop Relat Res. 1998;354:49-56.
- Chauhan S.K., Scott R.G., Breidahl W., et al.: Computer-assisted knee arthroplasty versus a conventional jig-based technique. A randomised, prospective trial. J Bone Joint Surg Br. 2004;86:372-377.
- Bae D.K., Song S.J.: Computer assisted navigation in Knee arthroplasty. Clin Orthop Surg. 2011;3(4):259-267.
- Slamin J., Parsley B.: Evolution of customization design for total knee arthroplasty. Curr Rev Musculoskelet Med. 2012;5(4):290-295.
- Sassoon A., Nam D., Nunley R., et al.: Systematic review of patient-specific instrumentation in total knee arthroplasty: new but not improved. Clin Orthop Relat Res. 2015;473(1):151-158.
- Thienpont E., Schwab P.E., Fennema P.: A systematic review and meta-analysis of patient-specific instrumentation for improving alignment of the components in total knee replacement. Bone Joint J. 2014;96-B:1052-1061.
- Boonen B., Schotanus M.G., Kerens B., et al.: Intra-operative results and radiological outcome of conventional and patient-specific surgery in total knee arthroplasty: a multicentre, randomised controlled trial. Knee Surg Sports Traumatol Arthrosc. 2013;21(10):2206-2212.
- Kotela A., Lorkowski J., Kucharzewski M.: Patient-specific CT-based instrumentation versus conventional instrumentation in total knee arthroplasty: A prospective randomized controlled study on clinical outcomes and In-hospital data. Biomed Res Int. 2015;165908:8.




 Journal of Orthopaedics Trauma Surgery and Related Research a publication of Polish Society, is a peer-reviewed online journal with quaterly print on demand compilation of issues published.
Journal of Orthopaedics Trauma Surgery and Related Research a publication of Polish Society, is a peer-reviewed online journal with quaterly print on demand compilation of issues published.