Constitutional and Ossein-Primary Bone Lymphoma
Received: 11-Feb-2023, Manuscript No. jotsrr-23-88929; Editor assigned: 12-Feb-2023, Pre QC No. jotsrr-23- 88929 (PQ); Accepted Date: Mar 24, 2023 ; Reviewed: 17-Feb-2023 QC No. jotsrr-23- 88929 (Q); Revised: 23-Feb-2023, Manuscript No. jotsrr-23- 88929 (R); Published: 26-Mar-2023
This open-access article is distributed under the terms of the Creative Commons Attribution Non-Commercial License (CC BY-NC) (http://creativecommons.org/licenses/by-nc/4.0/), which permits reuse, distribution and reproduction of the article, provided that the original work is properly cited and the reuse is restricted to noncommercial purposes. For commercial reuse, contact reprints@pulsus.com
Introduction
Primary Bone Lymphoma (PBL) is an infrequently discerned manifestation of malignant lymphoma, in contrast to secondary lesions arising due to disseminated lymphoma. Primary bone lymphoma arises within skeletal system or diverse osseous sites. Primary bone lymphoma is defined as occurrence of lymphoma confined to a singular bone in the absence of distant dissemination for six months following initial disease discernment. Additionally, Primary Bone Lymphoma (PBL) is designated as a lymphoma emerging within an osseous site with absence of disease at diverse sites for minimally six months. Primary bone lymphoma may be accompanied by incrimination of regional lymph nodes. Multifocal primary bone lymphoma is uncommon and generally manifests with lymphoma confined to ≥ 2 bones accompanied by lack of distant neoplastic dissemination for six months. Primary bone lymphoma is frequently associated with soft tissue tumefaction. An estimated 40% of bone tumours are comprised of haematological neoplasms as plasma cell myeloma or lymphoma. Appropriate discernment of primary bone lymphoma may be challenging due to factors such as quantifiable tissue sample, focal fibrosis, commingling of miniature cells and crush artefacts.
Primary bone lymphoma configures<5% of extra-nodal lymphomas, <5% of various bone tumours and <1% of nonHodgkin’s lymphoma. Primary bone lymphoma commonly arises within adults with peak incidence within fifth decade to sixth decade and mean age of disease occurrence at 48 years although no age of disease emergence is exempt. Paediatric population below<10 years is exceptionally incriminated.
A mild male predominance is observed with male to female proportion of 1.5:1 [1, 2].
Majority (~80%) of primary bone lymphomas are configured by diffuse large B cell lymphoma.
Primary bone lymphoma is categorized a
• Group 1 comprised of solitary bone lymphoma.
• Group 2 constituted of multifocal bony lesion.
• Group 3 delineating instances with incrimination of distant lymph nodes.
• Group 4 demonstrating lymphoma associated withvisceral disease.
In contrast to primary bone lymphoma, secondary involvement of bone by lymphoma is commonly discerned and configures stage IV disease. Primary bone lymphoma can be appropriately staged with Ann Arbor staging of non-Hodgkin’s lymphoma [1]. Generally, primary bone lymphoma emerges within sites such as bone marrow, axial skeleton or vertebral column and femur although no site of disease emergence is exempt. Primary bone lymphoma frequently incriminates bony metaphysis although disease occurrence within diaphysis or epiphysis is indicative of progressive disease [2]. Of obscure aetiology, primary bone lymphoma incriminating the bone marrow is posited to occur due to contributory factors as osteoclast activating factor. Significant tumour dissemination and disease relapse is contingent to homing properties of lymphoma cells. Upon flow cytometry, clonal rearrangement of neoplastic lymphocytes aids in determining cellular phenotype.
Neoplastic lymphocytes depict clonal rearrangement of immunoglobulin genes as BCL2, BCL6 or MYC and appear non-reactive to Epstein Barr virus. Majority (~80%) of primary bone non- Hodkins lymphoma delineate chromosomal abnormalities. Primary bone lymphoma manifests preponderantly with localized bone pain, a palpable tumefaction, pathological fracture and cogent neurological symptoms with incrimination of spinal canal and cord compression. Serum Lactate Dehydrogenase (LDH) levels may be elevated. B clinical symptoms as pyrexia, night sweats and >10% loss of body weight are uncommonly discerned [2, 3]. Primary bone lymphoma may relapse and incriminate diverse bones, regional lymph nodes, abutting soft tissue, pulmonary parenchyma, bone marrow or Central Nervous System (CNS). Cytological examination delineates a varying combination of centroblasts and immunoblasts. Enlarged, bizarre cells may be discerned. Peripheral blood film exceptionally depicts neoplastic lymphoma cells whereas centroblasts appear as enlarged, pleomorphic cells imbued with abundant cytoplasm, lobulated nucleus and ≥ one prominent nucleoli [2, 3].
Generally, miniature tissue samples are obtained in order to circumvent disabilities due to pathological fracture.
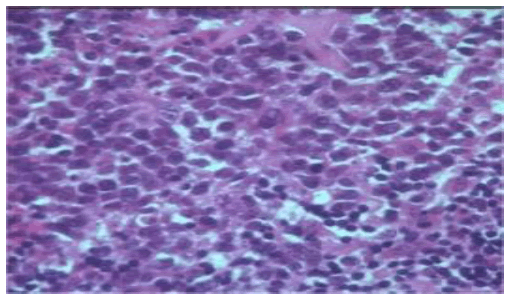
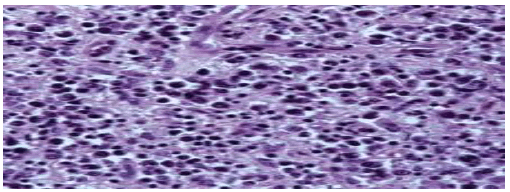
Upon gross examination, characteristic ‘fish flesh’ appearance of lymphoma is encountered. Extra-osseous tumour extension and an indistinct tumour perimeter are observed. Upon microscopy, diffuse large B cell lymphoma is commonly (~80%) discerned wherein cellular morphology appearing at diverse sites such as diffuse pattern of tumour configuration and neoplastic infiltration between bone trabeculae is identical [2, 3].
Lymphoma is composed of enlarged, atypical lymphoid cells permeated with abundant cytoplasm, clumped nuclear chromatin and prominent nucleoli and appear admixed with centroblasts, immunoblasts, enlarged, bizarre cells and a component of miniature lymphocytes. Prominent foci of spindle-shaped cells and fibrosis are observed.
Additionally, primary bone lymphoma may be constituted of variants such as Burkitt’s lymphoma, lymphoblastic lymphoma, follicular lymphoma, low grade B cell lymphoma, various T cell lymphomas and Hodgkin’s lymphoma. Diffuse Large B Cell Lymphoma (DLBCL) is a frequent subtype of primary bone lymphoma implicating bony pelvis and femur. Besides, implicated adults demonstrate neoplastic emergence commonly confined to regions of persistent red marrow [2, 3].
Upon ultrastructural examination, centroblasts demonstrates cleaved nuclei whereas immunoblasts are pervaded with enlarged, spherical nuclei, coarse chromatin and 1 to 3 prominent nucleoli. Rough endoplasmic reticulum, dilated cisternae and prominent Golgi apparatus are exemplified. Occurrence of aforesaid features are contingent to proportionate plasmacytoid differentiation [2, 3] (Fig. 1 and 2).
Primary bone lymphoma is immune reactive to CD30, CD45 and Anaplastic Lymphoma Kinase (ALK) whereas immune reactivity to B cell markers and T cell markers are contingent to diverse subtypes of emergent lymphoma. Diffuse large B cell lymphoma can delineate germinal centre phenotype with CD10+, BCL2+ immuno-phenotype, post-germinal centre phenotype with CD10−, BCL2− immuno-phenotype or an undetermined phenotype. Primary bone lymphoma is immune non-reactive to CD99, diverse neuroendocrine markers, cytokeratin or S100 protein [3,4]. Primary bone lymphoma requires segregation from neoplasms such as metastatic carcinoma, osteosarcoma, reactive inflammatory disorders, spindle cell sarcoma, poorly differentiated plasmacytoma or myeloid sarcoma, various round blue cell tumours of bone, neuroectodermal tumour, metastatic neuroblastoma, osteosarcoma- small cell variant, mesenchymal chondrosarcoma or metastatic small cell carcinoma. Upon plain radiography, segregation is required from lesions demonstrating permeation of bony trabeculae with bone destruction as infection, eosinophilic granuloma, Ewing’s sarcoma or metastasis from various primaries into skeletal system. Primary bone sarcoma can be appropriately discerned with cogent clinical and radiological features confirmed with surgical tissue sampling. Primary bone lymphoma demonstrates elevated levels of serum Lactate Dehydrogenase (LDH) and β2 micro-globulin. Complete Blood Count (CBC), Erythrocyte Sedimentation Rate (ESR) and C-Reactive Protein (CRP) require evaluation (3,4). Radiographic examination depicts a neoplasm predominantly permeating inter-trabecular spaces with configuration of commingled lytic and sclerotic bone lesions. Generally, primary bone lymphoma incriminates a significant expanse of bone wherein lesions may be uni-focal, monostotic or polyostotic. Bone cortex is damaged in the absence of configured periosteal, reactive new bone. Bony sclerosis is variable and admixed with cystic foci. Incrimination of regional lymph nodes and circumscribing soft tissue is common. Upon plain radiography, primary bone lymphoma demonstrates non-specific features wherein affected bone may be normal or displays lytic lesions, lesions with peripheral sclerosis or a mixed configuration. The commonly discerned lytic lesions are associated with permeative bone destruction along with broad zone of transition from normal to neoplastic bone. Thickening of bony cortex and periosteal reaction may be exemplified. Magnetic Resonance Imaging (MRI) delineates signal abnormalities confined to bone marrow. Upon T1 weighted imaging, bone marrow demonstrates minimal signal intensity. Upon T2 weighted imaging, bone marrow enunciates elevated signal intensity [3, 4]. Primary bone lymphoma is appropriately treated with a combination of radiotherapy and chemotherapy. Few instances may be subjected to surgical intervention as the modality may delay commencement of chemotherapy.
Singular chemotherapy is recommended for treating paediatric primary bone lymphoma and is associated with superior therapeutic response. Employment of radiotherapy may engender bone sarcoma. Primary bone lymphoma demonstrates superior prognostic outcomes with 5 year proportionate survival > 80% [3, 4].
Factors contributing to favourable prognostic outcomes are comprised of
• Polyostotic subtype of bone disease .
• Advanced disease stage .
• Age of incriminated subjects > 60 years.
• Disease emergence within mandible or maxilla .
• Elevated International Prognostic Index (IPI) score .
• Eastern Cooperative Oncology Group (ECOG) performance status.
• Normal serum lactate dehydrogenase (LDH) levels • Adoption of combined therapeutic modalities
• Enhanced dosage of radiation therapy
• >3 cycles of chemotherapy
•Non germinal centre phenotype of diffuse large B cell lymphoma[3, 4].
References
- Yang XY, He X, Zhao Y et al. Nomogram-Based Prediction of Overall and Cancer-Specific Survival in Patients with Primary Bone Diffuse Large B-Cell Lymphoma: A Population-Based Study. Evid.-Based Complement. Altern. Med. 2022;2022.
- Cunha G, Alçada M, Mestre A, et al. Primary Bone Lymphoma: A Rare Cause of Chronic Back Pain. Cureus. 2022;14(1).
- Ayesh Haj Yousef MH, Audat Z, Al-Shorafat DM, et al. Primary Diffuse Large B Cell Lymphoma of Bone: A Single-Center Experience. J. Blood Med. 2022:143-9.
- Muñoz N. Primary bone lymphoma: report of 7 cases. Med. Clin.,2018;151(10):421-2.2018;151(10):421–422.[GoogleScholar][CrossRef]



 Journal of Orthopaedics Trauma Surgery and Related Research a publication of Polish Society, is a peer-reviewed online journal with quaterly print on demand compilation of issues published.
Journal of Orthopaedics Trauma Surgery and Related Research a publication of Polish Society, is a peer-reviewed online journal with quaterly print on demand compilation of issues published.