Epiphyseal detachment fractures in patients and physical injuries in patients with spina bifida: About one case
Received: 30-Dec-2022, Manuscript No. jotsrr- 23-85294; Editor assigned: 06-Jan-2023, Pre QC No. jotsrr- 23-85294(PQ); Accepted Date: Jan 14, 2023 ; Reviewed: 08-Jan-2023 QC No. jotsrr- 23-85294(Q); Revised: 12-Jan-2023, Manuscript No. jotsrr- 23-85294(R); Published: 15-Jan-2023
This open-access article is distributed under the terms of the Creative Commons Attribution Non-Commercial License (CC BY-NC) (http://creativecommons.org/licenses/by-nc/4.0/), which permits reuse, distribution and reproduction of the article, provided that the original work is properly cited and the reuse is restricted to noncommercial purposes. For commercial reuse, contact reprints@pulsus.com
Abstract
Background: Epiphyseal detachment fractures of the distal end of the femur are relatively common in patients with spinabifida, but they most often go unnoticed due to sensory disturbances and/or minimal displacement of the fractures in this type of patient. These patients present with a hot tumefaction of the knee often with general inflammatory signs, but without pain or notion of trauma. We report a case of epiphyseal detachment fracture of the distal end of the femur in a 06-year-old child with myelomeningocele. Distal femoral physical injuries are relatively common in patients suffering from spina bifida; but often go unnoticed due to lack of sensitivity and/or the minimally displacement of fractures in this case of patients. These patients present with warmth swollen knee with often inflammatory signs, with no known history of trauma or pain. We report the case of physical injury of distal femur in a 6-year-old child with myelomeningocele.
Keywords
Epiphyseal detachment, spina bifida, knee swelling, physical injuries, spina bifida, swollen knee
Introduction
Epiphyseal detachment fractures in patients with myelomeningocele are common complications [1, 2]. T hey are due to sensory disorders and osteoporosis. T hey occur in 10% to 30% of patients, with knee involvement in 50% of cases [1,3].
These fractures generally manifest themselves in the form of a hot tumefaction with sometimes fever and hyperleucocytosis [1-3]. T hey are rarely painful and without notion of trauma [2].
An infection (arthritis, osteomyelitis), or even a sarcoma can be evoked, which delays the diagnosis of the fracture [3, 4].
Case Presentation
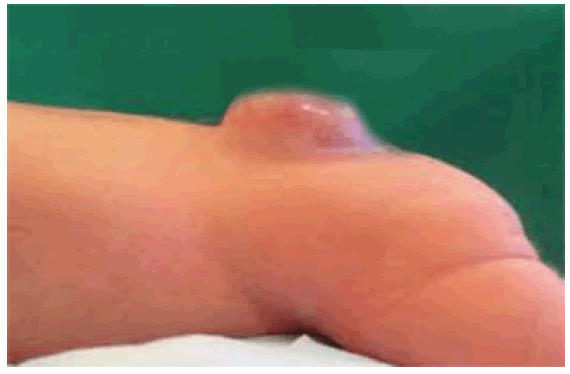
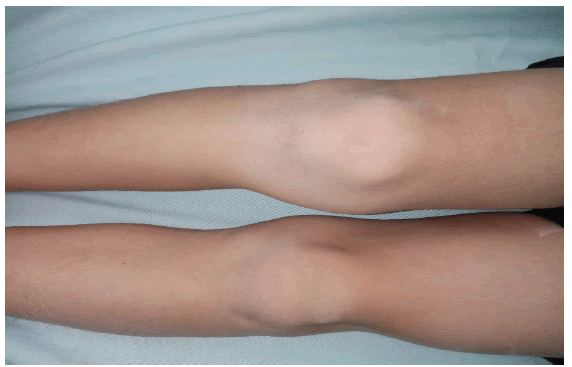
Our 6-year-old male patient, carrier of myelomeningocele (Fig.1), and not walking, was hospitalized urgently at the level of the pediatric department for a painless hot swelling of the left knee without notion of trauma and without deformation visible from the knees (Fig. 2), with Hyper leukocytosis. The diagnosis of acute osteoarthritis of the knee was suspected and the patient was put on double intravenous antibiotic therapy.
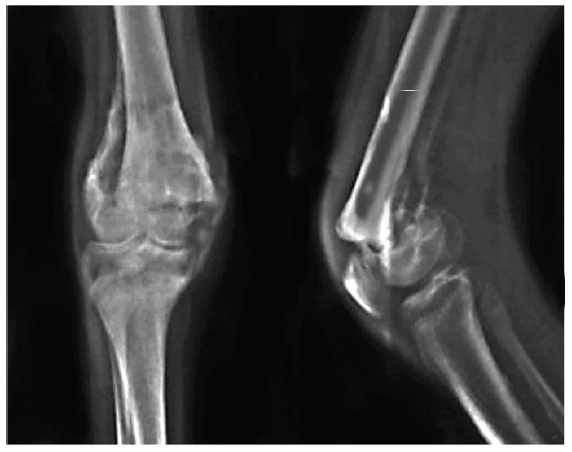
On the 7th day of his hospitalization, a conventional x-ray of both knees was taken which showed an epiphyseal detachment fracture in the process of consolidation of the distal end of the femur (Fig. 3).
Our treatment was immobilization of the left lower limb with a cruropedial cast for 1 month.
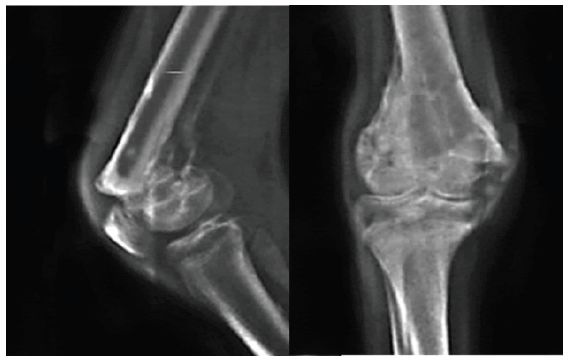
The radio-clinical evolution after one month of immobilization was marked by the disappearance of the swelling of the knee with a consolidation of the fracture and the formation of a hypertrophic callus (Fig. 4).
Discussion
In children with spina bifida, the most common fractures are epiphyseal fractures of the femur [3, 4], and the side most affected is the one with sensory disorders [1].
The diagnosis of the fracture must always be evoked in front of any warm swelling [1, 2]. Most often there is no notion of direct violent trauma in these patients, moreover one can find the notion of ordinary repeated trauma (falls, aggressive manipulation of the limbs, etc.) [2].
The radiological changes observed in these patients (hypertrophic callus) and the presence of inflammatory signs may evoke other diagnoses (osteomyelitis, osteosarcoma, etc.), and lead to unnecessary procedures such as puncture and biopsy [1, 3, 4].
The treatment of these fractures consists of immediate plaster immobilization to prevent displacement of the fracture and its consolidation into a malunion [2], and the duration of immobilization should be short so as not to aggravate osteoporosis and avoid stiffness articular.
Conclusion
Children with myelomeningocele have a potential risk of fracture of the lower limbs due to osteoporosis and sensory disturbances. These fractures can often go unnoticed.
It is important to know the clinical and radiological aspect of fractures in this type of patient in order to proceed with appropriate treatment and avoid unnecessary additional examinations.
Conflicts of Interest
No conflict of interest is declared
References
- Khoury JG, Morcuende JA. Dramatic subperiosteal bone formation following physeal injury in patients with myelomeningocele. Iowa orthop j. 2002; 22:94. [Google Scholar]
- Roberts JA, Bennet GC, MacKenzie JR. Physeal widening in children with myelomeningocele. J Bone Jt Surg. British volume. 1989 Jan; 71(1):30-2. [Google Scholar]
[CrossRef]
- Cuxart A, Iborra J, Melendez M. Physeal injuries in myelomeningocele patients. Spinal Cord. 1992 Nov; 30(11):791-4. [Google Scholar]
[CrossRef]
- Asirdizer M, Zeyfeoglu Y. Femoral and tibial fractures in a child with myelomeningocele. J Clin Forensic Med. 2005 Apr 1; 12(2):93-7. [Google Scholar]
[CrossRef]



 Journal of Orthopaedics Trauma Surgery and Related Research a publication of Polish Society, is a peer-reviewed online journal with quaterly print on demand compilation of issues published.
Journal of Orthopaedics Trauma Surgery and Related Research a publication of Polish Society, is a peer-reviewed online journal with quaterly print on demand compilation of issues published.