Ipsilateral concomitant displaced vertical femoral neck fracture and unstable 4-part trochanteric fracture: A case report
Received: 24-Oct-2018 Accepted Date: Jan 08, 2019 ; Published: 15-Jan-2019
This open-access article is distributed under the terms of the Creative Commons Attribution Non-Commercial License (CC BY-NC) (http://creativecommons.org/licenses/by-nc/4.0/), which permits reuse, distribution and reproduction of the article, provided that the original work is properly cited and the reuse is restricted to noncommercial purposes. For commercial reuse, contact reprints@pulsus.com
Abstract
Concomitant displaced vertical neck fracture and unstable 4-part trochanteric fracture in the ipsilateral femur has seen rarely but they can occur on occasions. One such case was seen a 56-year-old male patient with both of those fractures. He underwent dynamic hip screw fixation for intertrochanteric and neck fracture with a candy- packing wiring for reduction of lesser trochanteric fragment. At the 18th month follow-up after surgery, all fracture sites were united with no evidence of avascular necrosis of the femoral head on radiograph and the function of the hip joint was restored without pain. We would report this case with a review of the literature; the anatomical reduction and stable internal fixation are an important factor for a good prognosis in a young patient with concomitant displaced vertical neck fracture and unstable 4-part trochanteric fracture in the ipsilateral femur.
Keywords
Intertrochanteric fracture, neck fracture, dynamic hip screw, candy-packing wiring, concomitant fracture, ipsilateral femurIntroduction
It is very rare that neck and intertrochanteric fractures occur simultaneously in the ipsilateral femur. Simultaneous intertrochanteric fracture and un-displaced neck fracture in the ipsilateral femur accompanied with osteoporosis were reported rarely in the elderly patients. Most of them were un-displaced subcapital femoral neck fractures found during or after fixation [1]. In patients with good bone quality, a femoral neck fracture accompanied by an intertrochanteric fracture is extremely rare. We had experienced a 56-year-old male patient with the concomitant displaced vertical neck fracture and unstable 4-part trochanteric fracture in the ipsilateral femur after fell. He underwent a dynamic hip screw fixation to the intertrochanteric and neck fracture with candy-packing wiring that provides posteromedial cortical stability for reduction of lesser trochanteric fragment.
The bone was successfully united without notable deformities at fracture site and the clinical outcome at the 18th-month follow-up was excellent, we report this case with review of the literature in terms of rarity and discuss the injury mechanism and an effective method of fixation. The patient was informed that medical data concerning the case would be submitted for publication and provide consent.
Case Report
A 56-year-old male patient fell from a height of 2 m during construction work. At the time of transfer to emergency room, the proximal thigh was swollen, tenderness at hip was remarkable and there were no signs of neurological abnormalities or vascular injuries.
On plain radiograph showed AO/OTA classification A2.3 femoral intertrochanteric fracture and Pauwel classification type III vertical femoral neck fracture. A 3D computed tomography images showed an unstable four-part fracture at the intertrochanteric region with fragments of the lesser and greater trochanter and vertically running femoral neck fracture (Fig. 1). The fragments of the intertrochanteric region were comminuted but the neck fracture was not displaced severely. Concerning the patient’s age and activity level, open reduction and internal fixation were performed at 8 hours later after the trauma.
Figure 1: Preoperative X-ray of the left hip with simultaneous intertrochanteric and femur neck fracture. A,B: anteroposterior and axial radiograph showing vertical femur neck and AO/OTA 2.3 type intertrochanteric fracture. C: Three dimensional computed tomography image showing comminuted intertrochanteric fracture at great trochanter and lesser trochanter
After positioning the patient in supine position on the fracture operation table, reduce the fracture site through traction and rotation. The state of reduction was checked under the image intensifier but it was unacceptable. We had done proximal femoral lateral incision approximately 10 cm in length after then dissect the vastus lateralis fascia at the trochanteric ridge with L-shape configuration to palpate the trochanteric fracture site and anterior capsulotomy to palpate the fracture line of the femoral neck and the lesser trochanter with a limited modified Watson-Jones approach. The femur was applied traction to longitudinal direction and the external rotation controlled by an image intensifier and reduced the intertrochanteric main fracture segments.
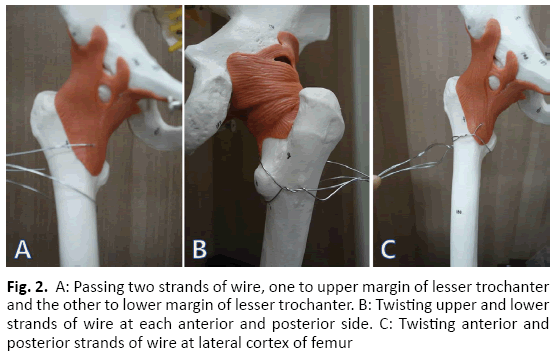
The lesser trochanteric fragment was preliminary reduced by cerclage passer under the image intensifier with indirect reduction technique and fixed using candy-packing wiring technique, passing two strands of wire (#7; Synthes, West Chester, PA, USA) to the upper and lower border of adhering part of the iliopsoas tendon using cerclage passer. Then twisted anterior two wires and pull the two wires inferiorly to fasten the lesser trochanter fragment to the posteromedial cortex. After then twisted the posterior two wire and making a candy packing like wire ring that was placed between the psoas tendon and lesser trochanter fragment so that when the wires pulled together, the fragment could be adjusted to the posteromedial cortex (Fig. 2). To reduce the soft tissue destruction of the fracture site, the cerclage passer was passed to the upper and lower margins of the lesser trochanter fragment assisted by the image intensifier. We could get the anatomical reduction of the lesser trochanteric fragment. The greater trochanter was temporarily fixed using K-wire after reduction.
After insertion of the K-wire into the femoral head at the capsulotomy site, the neck fracture was rotationally aligned by joy stick technique. Then preliminary fixation to the neck fracture was done using two Steinmann pins. Simultaneous fixation of the intertrochanteric and neck fractures was performed by using dynamic hip screw (DHS; Synthes, West Chester, PA, USA). The greater trochanter was fixed using a figure of eight-wire loop technique. Amount of the blood loss during operation was estimated by count of the gauze and suction bottle, it was check by 450 ml. Post-operative blood loss was estimated by count of the suction drain tube bag for two days after surgery, it was checked by 300 ml.
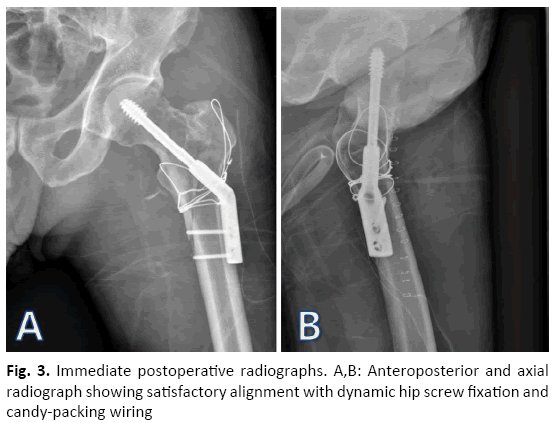
Postoperative radiographs showed anatomical reductions of both the femoral neck and the intertrochanteric fracture sites. Garden’s alignment index of the femoral neck was in the normal range and neck-shaft angle was 130Ëš (Fig. 3).
Surgical wound was healed clearly by 10 days after operation and there were no wound infection and skin necrosis. Laboratory findings such as Erythrocyte Sedimentation Ratio (ESR) and C-Reactive Protein (CRP) were normalized by 2 weeks after operation.
Passive joint exercise was initiated in the bed after confirming the disappearance of acute pain on the second day after surgery. After 6 weeks of partial weight bearing postoperatively, gradual increasing of weight bearing was performed after confirming the fracture site consolidation by periodic radiographic examination for 6 weeks. Three months after the operation, total weight bearing was performed.
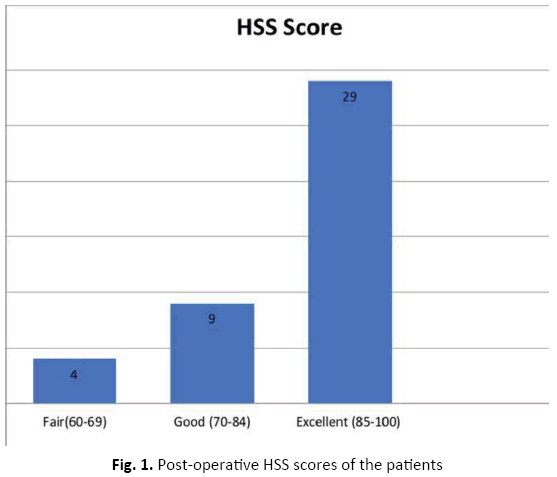
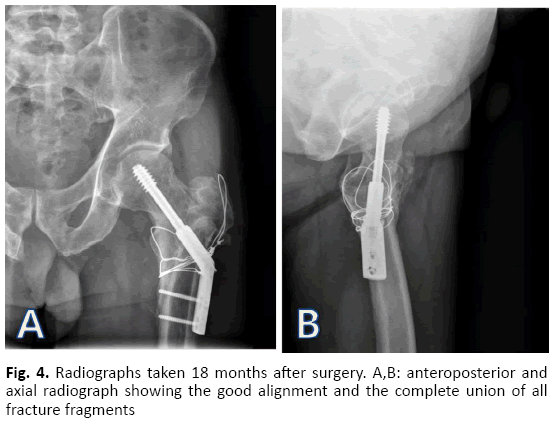
Bone union was confirmed radiologically four months after surgery without notable deformities at the fracture site. At the 18th-months follow-up, the intertrochanteric and the neck fractures were united without osteonecrosis of the femoral head (Fig. 4). Except for intermittent discomfort in the lateral thigh, there was neither limping gait nor other pain. As for the functional outcomes, Harris hip score and Parker and Palmer mobility score were checked at the last follow-up, 90 points and 9 points respectively.
Discussion
Femoral shaft fractures have been the most common fracture associated with the ipsilateral femoral neck fracture, but a concomitant intertrochanteric fracture was associated rarely [2]. There are twelve reports in the medical literature on ipsilateral fractures of the femoral neck and intertrochanteric regions. Most of them were intertrochanteric fractures accompanied with undisplaced neck fractures in the ipsilateral femur in the elderly associated with osteoporosis [3]. Devdatta et al., report a case of bony union treated with a dynamic condylar screw and a cannulated screw in a reverse oblique shape intertrochanteric fracture accompanied with a femoral neck fracture [3].
Generally, the femoral neck fractures in high energy injuries are caused by the transfer of external forces along the long axis of the femur [4]. However, in our presented case, judging by the morphology of the vertical femoral neck fracture and the four parts unstable type intertrochanteric fracture, we assumed injury mechanism that initially, the direct impact applied to the lateral part of the intertrochanteric region caused the unstable intertrochanteric fracture, followed by comminuted fragments of proximal part were extended to the femoral neck fracture by rotational force.
An unstable intertrochanteric fracture is usually accompanied with posterior cortex fragments including lesser trochanter, and comminuted greater trochanter fragments. It is known that internal fixation using with a cephalomedullary nail is biomechanically and structurally more stable than a dynamic hip screw fixation [5]; however, there are no reports about accompanying femoral neck fractures. Cohen et al., reported excellent result in fixation using a dynamic hip screw to the intertrochanteric fracture associated with un-displaced femoral neck fracture [1].
Baitner et al., reported that fixation with a dynamic hip screw prevents downward displacement of the femoral head and reduces the shearing force of the fracture site when the inclination of the femoral neck fracture line is steep therefore, decreases the probability of failures [6]. Weber et al., suggested that the use of an anti-rotation cannulated screw and a dynamic hip screw is the most stable but, using a dynamic hip screw must be limited since there is a risk of obstruction of the head’s blood flow by reaming of large diameter [7].
In this case, the internal fixation with a dynamic hip screw was done to decrease the shearing force to the vertical femoral neck fracture site and to gain stable fixation of the intertrochanteric fracture site, simultaneously. Although the dynamic hip screw is still widely used for the treatment of intertrochanteric fractures, it has high failure rate due to fixation failure or excessive gliding in case of the posteromedial cortex and lateral cortical buttress were comminuted [5].
There are a few reports to reserch of the optimal length of the side barrel plate, Yian et al., reported that 2-holes side plate fixation also optimal to obtain the stability of the fracture site in unstable trochanteric fracture treatment if there was no problem with the sliding of the lag screw [8].
McLoughlin et al., reported that there was no difference of 2-hole side plate and 4-hole side plate in terms of the screw breakage and amount of shearing force at the fracture site by mechanical experiment [9].
The basic concept of the DHS is the conversion of the axial loading to compression of the fracture site, we had been used 2-hole side plate for fixation of the AO/OTA type A1 and A2 trochanteric fractures to reduce soft tissue dissection and blood loss if the stable apposition of the medial cortex was obtained. In this case, we used 2-hole side plate to reduce soft tissue destruction and operation time after confirmation of the stable apposition of the fracture sites.
We considered that to obtain the anatomical reduction of the neck fracture site, anatomical reduction of the posteromedial cortex must be preceded in case of concomitant femoral neck and intertrochanteric fracture. Therefore, we performed an anatomical reduction of the lesser trochanteric fragment using a candy packing wiring technique, followed by the fixation of greater trochanter fragment using a figure of eight-shaped wiring technique to convert the intertrochanteric displaced four parts fracture into the form of two parts fracture after then final fixation was performed.
Lee et al., had reported the candy packing wiring technique that provides posteromedial stability including the lesser trochanter fragment in unstable intertrochanteric fractures [10]. Candy packing wiring technique is a useful fixation method when lesser trochanter fragment must be reduced anatomically.
The meticulous analyzes anatomical features of the fracture pattern and selects the appropriate fixation methods that should be helpful to prevent nonunion and fixation failure in the treatment of the concomitant displaced neck and intertrochanteric fracture treatment.
Conclusion
The concomitant displaced neck and intertrochanteric fractures in the ipsilateral femur in a young patient are very rare. There are few reports similar to this presented case in the past. Due to the high rate of nonunion in the vertical neck fractures and fixation failure in the unstable intertrochanter fractures, it is a challenge to try to osteosynthesis in case of complex fracture such as this case. So, we presumed that careful access to the fracture pattern and select the adjust fixation methods are the most important factors to succeed the osteosynthesis.
REFERENCES
- Cohen I., Rzetenly V.: Simultaneous ipsilateral pertrochanteric and subcapital fracture. Orthopedics. 1999;22(5):535-536.
- Seyegh F., Karataglis D., Trapotsis S., et al.: Concomitant ipsilateral pertrochanteric and subcapital fracture of the proximal femur. Eur J Trauma. 2005;31:64-67.
- Devdatta S.N., Kumar K.V., Trikha V., et al.: Ipsilateral femoral neck and trochanter fracture. Indian J Orthop. 2011;45:82-86.
- Haidukewych G.J., Rothwell W.S., Jacofsky D.J. et al.: Operative treatment of femoral neck fractures in patients between the age of fifteen and fifty years. J Bone Joint Surg Am. 2004;86:1711-1716.
- Kaplan K., Miyamoto R., Levine B.R., et al.: Surgical management of hip fracture: an evidence base review of literature. II: Intertrochanteric fractures. J Am Acad Orthop Surg. 2008;16:665-673.
- Baitner A.C., Maurer S.G., Hickey D.G., et al.: Vertical shear fractures of the femur neck: A biomechanical study. Clin Orthop Relat Res. 1999;367:300-305.
- Weber A.T., Bonnaire F.A.: Analysis of fracture gap changes: Dynamic and static stability of difference osteosynthesis procedures in the femoral neck. Injury. 2002;33:24-32.
- Yian E.H., Banerji I., Mattrews L.S.: Optimal side plate fixation for unstable intertrochanteric hip fractures. J Orthop Trauma, 1997;11:254-259.
- McLoughlin S.W., Wheeler D.L., Rider J. et al.: Biomechanical evaluation of the dynamic hip screw with two-and four- hole side plate. J Orthop Trauma. 2000;14:318-323.
- Lee J.M., Lee J.H., Lee C.W., et al.: New wiring for lesser trochanter fixation in unstable intertrochanteric fractures. J Korean Fract Soc. 2005;18:209-212.



 Journal of Orthopaedics Trauma Surgery and Related Research a publication of Polish Society, is a peer-reviewed online journal with quaterly print on demand compilation of issues published.
Journal of Orthopaedics Trauma Surgery and Related Research a publication of Polish Society, is a peer-reviewed online journal with quaterly print on demand compilation of issues published.