Outcome and challenges of management of limb length discrepancy using linear rail system
Received: 15-Jun-2017 Accepted Date: Aug 21, 2017 ; Published: 24-Aug-2017
This open-access article is distributed under the terms of the Creative Commons Attribution Non-Commercial License (CC BY-NC) (http://creativecommons.org/licenses/by-nc/4.0/), which permits reuse, distribution and reproduction of the article, provided that the original work is properly cited and the reuse is restricted to noncommercial purposes. For commercial reuse, contact reprints@pulsus.com
Abstract
Background: Management of limb length discrepancy (LLD) is a rewarding procedure though time consuming and is associated with some challenges. The aim of this study was to determine the time it takes for complete treatment of LLD from the time of osteotomy, with respect to the length of the LLD, method used, types of bone involved, pathologies and site of osteotomy.
Method: All consecutive patients with LLD more than 4 cm who consented during the study period were recruited into the study. Data obtained was analysed using SPSS version 19.
Results: Twenty-three patients were recruited into the study, 18 males and 5 females. The mean age was 36.35 ± 7.87 years, ranged 25–50 years. The mean LLD corrected was 7.30 ± 1.19 cm (range 5 cm to 9 cm). There were 12 tibia (52.2%) and 11 femur (47.8%), infective pathologies were 15 (65.2%), while non infective pathologies were 8 (34.8%). Bone transport was done in 8 (34.8%) patients while bone lengthening was done in 15 (65.2%) patients. Diaphyseal osteotomy was done in 13 (56.5%) patients while metaphyseal osteotomy was done in 10 (43.5%) patients. The mean time from osteotomy to removal of LRS was 264.39 ± 53.65 days. The complications noticed were pin tract infections, residual LLD, angulation of regenerate, and delayed union at ducking site.
Conclusion: LRS produces good outcome in the management of LLD for both infective and non-infective pathologies, with osteotomy done at metaphysis or diaphysis using either bone transport or bone lengthening methods.
Keywords
Osteotomy, Regenerate, Pathologies
Introduction
Limb equality is of great important especially in the lower limbs for normal gait and curvature of the spine. When there is limb length discrepancy (LLD) in the lower limbs, walking becomes difficult, the pelvis becomes tilted to one side with resultant curvature of the spine (scoliosis) and associated low back pain. All these make treatment of LLD very important [1,2].
LLD may be caused by congenital defects such as shortening of bones, absence of bone, or bone dysplasias. It may also result from trauma, such as gunshot injury or bone loss following road traffic injury. LLD can also result following resection of dead or infected bone [3,4]. Other causes of LLD in the lower limbs which require treatment of the primary problems rather than correction of the discrepancy alone include malunited fractures, avascular necrosis of head of femur, and perthe’s disease.
Limb discrepancies of less than 4 cm may be treated with shoe raise; whereas LLD of 5 cm to 12 cm may be treated with vascularised bone grafts where the skill is available [5]. Bone transport or bone lengthening are widely acceptable procedures used for treatment of LLD of 2 cm to 10 cm [5]. Ilizarov method was initially introduced for bone transport and bone lengthening, but the device is too cumbersome for patients, expensive, and highly technical. The Linear Rail System (LRS) is a form of external method for LLD correction which has been widely accepted because it is less cumbersome for patients to carry, less expensive, and its outcome has been shown to be as good as the Ilizarov method [6-8] (Figure 1).
The aim of this study was to determine the time it takes for complete treatment of LLD from the time of osteotomy, with respect to the length of the limb discrepancy being corrected. And also, to compare the outcome in patients with both infective and noninfective pathologies. This may enable better patient counseling and preparation before the procedure.
Methodology
This is prospective study done at Federal Medical centre, Birnin Kebbi, Nigeria. From May 2014 to April 2016. All consecutive patients that had bone gaps or limb length discrepancy (LLD) of more than 4 cm and those patients expected to have bone gaps or LLD of more than 4 cm following resection of a non-viable part of bone were recruited into the study after obtaining their consent.
Patients with 5 cm to 7 cm of LLD had bone lengthening. This involved apposition and compression of the freshened ends of bone (acute ducking), followed by osteotomy proximal or distal to the ducking site for lengthening. Those patients with LLD more than 7 cm had bone transport. Where in the gap in between the freshened ends of bone are not apposed. The gap is maintained with the LRS device followed by osteotomy proximal or distal to the gap. The segment of bone in between the gap and osteotomy site is distracted gradually (gradual ducking) to occlude the space.
The infectious cases had two staged procedure: the first stage was excision of infected part of the bone, removal of infected soft tissue, application of LRS, and control of infection with systemic antibiotics. The second stage involved osteotomy after resolution of infection. The noninfectious cases had application of LRS and osteotomy as a single staged procedure.
Following osteotomy, patients were taught how to turn the compression distraction unit of the LRS for distraction osteogenesis. Distraction usually commences by day 10-12 post osteotomy, at a rate of 1mm per day. The compression distraction unit is turned through 90° every 6 hours to give bone distraction distance of 0.25mm every 6 hours.
Patients stay on the ward for about a month after they have commenced distraction, to monitor them during the distraction process, and are subsequently discharged to continue the distraction at home. Follow up was carried out at 3 weekly intervals to monitor the bone regenerate with the aid of plain radiographs. Once adequate length of regenerate has been achieved, the distraction process was stopped, and patient was left with the LRS in place for a period which is about three times the period used to achieve the required length of the limb. This is to allow for consolidation of the regenerate. The LRS device was removed once there is tricortical radiographic consolidation on two orthogonal radiographs. Patients were commenced on partial weight bearing about a month before removing the LRS, and this continues until about 6 weeks after which full weight bearing may be commenced.
The data obtained were recorded in proforma, these were analyzed by SPSS version 19. The test of significant association was done by using Fisher exact test, the level of statistical significant was set at P<0.05.
Results
During the study period, 23 patients were recruited into the study, there were 18 males and 5 females, with M: F of 3.6: 1. The age range was 25-50 years with a mean age of 36.5 years. The femur was involved in 47.8% (n=11) of patients and tibia was involved in 52.2% (n=12) of patients. The mean length of limb discrepancies managed was 7.3 cm (range from 5 cm to 9 cm).
The aetiology of LLD found included post sequestrectomy bone gaps (n=3, 13.0%), bone gaps following resection of infected nonunion (n=12, 52.2%), atrophic nonunion (n=3, 13.0%), congenital tibia shortening (n=1, 4.4%), and congenital shortening of femur (n=1, 4.4%), and gunshot injuries (n=3, 13.0%).
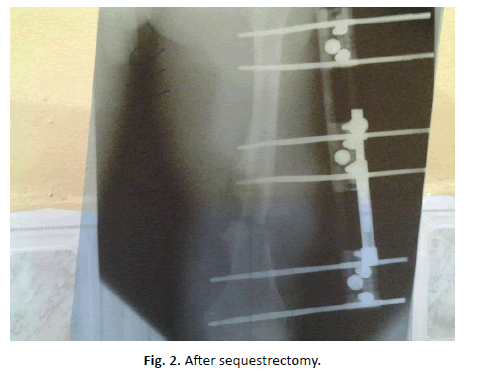
The mean limb length discrepancy treated was 7.30 ± 1.19 cm, (range 5 cm to 9 cm). The duration of hospital stay after osteotomy was 4–5 weeks, while the mean duration between the time of osteotomy and the time the LRS was removed was 264.39 ± 53.65 days, (range 161–360 days). However, those patients with infective pathologies had additional duration of 3–6 weeks between insertion of LRS and osteotomy (Table 1 and Figure 2).
| N | Age(Yrs) | Sex | LLD(cm) | Bone | Indications | Methods | Stages | Time from osteotomy to LRS removal (Days) | Complications |
|---|---|---|---|---|---|---|---|---|---|
| 1 | 25 | M | 9 | R. Femur | COSM | Transport | 2 | 350 | Pin tract infection |
| 2 | 48 | M | 7 | R. Tibia | Infected nonunion | Lengthening | 2 | 231 | -- |
| 3 | 37 | M | 6 | L. Tibia | Infected nonunion | Lengthening | 2 | 218 | -- |
| 4 | 40 | F | 7 | L. Tibia | Infected nonunion | Lengthening | 2 | 214 | -- |
| 5 | 30 | M | 7 | R. Femur | COSM | Lengthening | 2 | 288 | -- |
| 6 | 46 | M | 7 | R. Femur | Infected nonunion | Lengthening | 2 | 279 | -- |
| 7 | 38 | F | 8 | L. Femur | Infected nonunion | Transport | 2 | 290 | Pin tract infection |
| 8 | 26 | M | 6 | R. Tibia | Gunshot injury | Lengthening | 1 | 200 | -- |
| 9 | 30 | M | 7 | L. Femur | Infected nonunion | Lengthening | 2 | 290 | -- |
| 10 | 25 | F | 5 | R. Tibia | Congenital shortening | Lengthening | 1 | 165 | -- |
| 11 | 49 | M | 5 | R. Tibia | Atrophic nonunion | Lengthening | 1 | 161 | -- |
| 12 | 40 | M | 9 | R. Tibia | Infected nonunion | Transport | 2 | 279 | Regenerate angulation, 2cm LLD |
| 13 | 41 | M | 9 | L. Femur | Atrophic nonunion | Transport | 1 | 360 | Delayed union at ducking site |
| 14 | 38 | M | 7 | R. Femur | Infected nonunion | Lengthening | 2 | 290 | -- |
| 15 | 32 | M | 7 | R. Tibia | Infected nonunion | Lengthening | 2 | 233 | -- |
| 16 | 37 | M | 7 | L. Tibia | Gunshot injury | Lengthening | 1 | 220 | -- |
| 17 | 22 | F | 9 | R. Femur | Congenital shortening | Transport | 1 | 325 | 2cm LLD |
| 18 | 41 | M | 7 | R. Femur | Infected nonunion | Lengthening | 2 | 300 | Pin tract infection |
| 19 | 50 | M | 8 | R. Femur | Gunshot injury | Transport | 1 | 310 | -- |
| 20 | 32 | M | 9 | L. Tibia | COSM | Transport | 2 | 300 | -- |
| 21 | 35 | M | 8 | R. Tibia | Infected nonunion | Transport | 2 | 250 | -- |
| 22 | 40 | F | 7 | R. Femur | Infected nonunion | Lengthening | 2 | 295 | -- |
| 23 | 34 | M | 7 | L. Tibia | Atrophic nonunion | Lengthening | 1 | 233 | -- |
Table 1: Patients with infective pathologies had additional duration of 3–6 weeks between insertion of LRS and osteotomy.
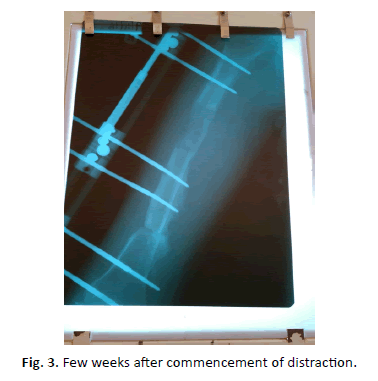
Bone transport was done for 34.8% (n=8) of patients whose LLD were more than 7 cm, while 65.2% (n=15) of the patients with LLD of 5 cm to 7 cm had bone lengthening done. The mean duration from time of osteotomy and removal of LRS from the patients are as shown in Table 2 and Figure 3.
| N | Variables | Mean time duration from osteotomy to LRS removal (days) | P-values |
|---|---|---|---|
| 1 | Methods | ||
| Bone transport | 295.50± 45.84 | P=0.002 | |
| Bone lengthening | 241.13± 46.78 | ||
| 2 | Pathologies | ||
| Infective | 373.80± 37.25 | P=0.151 | |
| Non-infective | 234.25± 68.84 | ||
| 3 | Bones | ||
| Femur | 307.00± 26.83 | P=0.178 | |
| Tibia | 225.33± 40.28 | ||
| 4 | Site of osteotomy | ||
| Diaphysis | 280.38± 45.89 | P=0.511 | |
| Metaphysis | 235.88± 57.11 | ||
Table 2: The mean duration from time of osteotomy and removal of LRS from the patients.
The outcome was without any complication in 69.6% (n=16) of patients. However, 13.0% (n=3) of patients had pin tract infection, 4.4% (n=1) of the patients had angulation of the regenerate, two (8.6%) of the patients had residual LLD of 2 cm each, and delayed union at the ducking site was noticed in 4.4% (n=1) of the patients.
Discussion
Correction of LLD is a time consuming, challenging and highly rewarding procedure. During the study period, 23 patients who required the procedure were recruited into the study; the mean age of these patients was 36.35 ± 7.87 years. This shows that the group of patients that require this procedure are the young adults, these are the people that constitute the work force of the country, hence the importance of this procedure.
There is male preponderance with a female to male ratio of 1: 3.6, the reason for this finding may be due to male being more involved in activities that makes them prone to trauma and violence. Dabkana et al. reported male preponderance in a similar study done in Maiduguri, Nigeria [9].
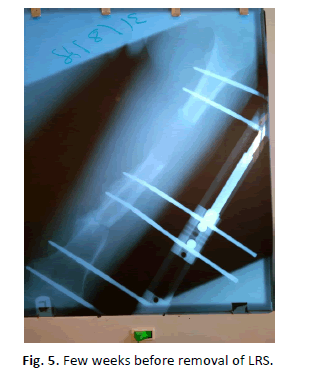
The mean duration of time from osteotomy and removal of LRS was more in the patients that had bone transport than those that had bone lengthening. This finding was statistically significant, (P<0.05). This may be because most patients who had bone lengthening had their osteotomy done at the diaphysis while majority of those patients who had bone transport had their osteotomy done at metaphyseal region where the force of distraction has been reported to be higher [10]. The time between osteotomy and removal of LRS on the patient was more in those patients who had diaphyseal osteotomy than those that had metaphyseal ostoetomy. (P>0.05). However, this finding contradicts the report of Aronso et al. where the duration was expected to be higher in those with metaphyseal osteotomy because of the reported higher distraction force required in this region [10] (Figures 4 and 5).
The patients with infective pathologies such as COSM, infected nonunion had two stages procedure, first stage was for debridement, application of LRS and control of infection, this usually takes about 3-6 weeks. The second stage was osteotomy after the infection has been controlled. Those patients with noninfective pathologies such as congenital shortening, atrophic nonunion and gunshot injury had application of LRS and osteotomy as a single stage procedure. The duration for stage one procedure make those patients with infective pathologies to have longer hospital stay than those with non-infective pathologies.
The commonest indication for the procedure was LLD following resection of infected nonunion (n=12), this was followed by LLD following sequestrectomy, resection of atrophic nonunion, and gunshot injury (n=3 each), then congenital shortening were two in number. All the infected nonunion managed were secondary to Traditional bone setters (TBS) management of closed fractures, none of them had medical co morbidity. This shows that there is need to create more awareness about the complication following management of fractures by TBS, so as to reduce these complications caused by them.
The commonest complication was pin tracts infection seen in 13.0% (n=3), all these three were patients that presented with infective pathologies. They were treated successfully with dressing around the point of entry of pin into the skin and antibiotics according to the sensitivity pattern of the organism growth. This was similar to the findings of Bari et al. where pin tract infection was the commonest complication noticed in their study [11]. Angulation of the regenerate was seen in a femur of a patient that had LLD of about 9 cm. Two patients had residual LLD of about 2 cm, this was corrected using shoe raise. There was delayed union at the docking site in one patient who had bone transport. Complications were seen in 6 patients, 5 out of which had the procedure on the femur. Previous studies have shown that the internal methods of limb lengthening have less complication than the external device, the internal methods is also more comfortable for patient than the external methods [12-15]. The technicality of the procedure for internal method of lengthening, the additional cost of surgery for removal of these device after lengthening has made the internal methods of lengthening less popular in this environment than the external method such as LRS used in this study [16].
The range of length of LLD corrected in the study was 5 cm to 9 cm, with a mean length of 7.30 cm ± 1.19 cm. Patients usually start partial weight bearing about a month prior to removal of LRS, so as to increase the strength of the regenerate, this continues till about 6 weeks after removal of LRS. All patients had satisfactory results because walking become better and easier with LLD correction. The major challenges were the high cost of treatment and long duration of time for carrying the LRS. The average cost of LLD correction using LRS device in this center is about two hundred and ten thousand naira (575 US dollar), the cost of device, investigations, admission and drug used inclusive. Although this may be considered very expensive by most patients in this environment, the importance of having ones LLD corrected surpasses the expenses of the procedure.
Conclusion
Distractive osteogenesis is a rewarding procedure though time consuming, LRS give good result for the procedure for both infective and non-infective pathologies, with osteotomy done at metaphysis or diaphysis using either bone transport or bone lengthening methods.
REFERENCES
- Defrin R., Ben Benyamin S., Aldubi RD., et al.: Conservative correction of leg – length discrepancies of 10mm or less for the relief chronic low back pain. Archives of Physical Medicine and Rehabilitation. 2005;86:2075-2080.
- Giles L.G., Taylor J.R.: Low back pain associated with leg length ineguality. Spine. 1981;6:510-521.
- Malimoud A.N., Arugad M., Abdel mohsen M.T., et al.: Is the intramedullary Skeletal Kinetic Distractor a Safe Measure For Bone Lengthening? A Systemic Review. J Orthop Trauma and Rehabilitation. 2004;18:69-78.
- Kesemenli C., Subasi M., Kirkgoz T., et al.: Treatment of traumatic bone defect by bone transport. ActaOrthopaedicBeldica. 2001;67:380-386.
- De Coster T.A., Gehlert R.J., Mikola E.A., et al.: Management of post-traumatic segmental bone defects. J AM Accad Orthop Surg. 2004;12:28-38.
- McCarthy J.J., MacEwen G.D.: Management of Leg Length Inequality. J South Orthop Assoc. 2001;10:73-85.
- Paley D., Maar D.C.: Ilizarov bone transport treatment for tibial defects. J Orthop Trauma. 2000;14:76-85.
- Rozbrunch S.R., Herzenberg J.E., Tetsworth K., et al.: Distraction Osteogenesis after high Tibia Osteotomy. ClinOrthopRelet Res. 2002;394:227-235.
- Dabkana T.M., Nyaku F.T., Bukar B.: Management of traumatic segmental bone loss using linear rail system., our experience at the University of Maiduguri Teaching Hospital, Maiduguri, Nigeria. Sahel Med J. 2016;19:171-174.
- Aronso J., Herp J.H.: Mechanical force as predictors of healing during Tibial lengthening by distraction osteogenesis. ClinOrthopRelat Res. 1994;301:73-79.
- Bari M.M., Shahidul I., Shetu N.H., et al.: Correction of Leg-Length Discrepancies by Ilizarov Technique. MOJ OrthopRheumatol. 2015;2:00029.
- Hamdy R.C., Bernstein M.A., Fragomen A.T., et al.: What's new in limb lengthening and deformity correction. J Bone Joint Surg Am. 2016;98-A:1408-1415.
- Paley D. PRECICE intramedullary limb lengthening system. Expert Rev Med Devices. 2015;12:231-249.
- Landge V., Shabtai L., Gesheff M., et al.: Patient satisfaction after limb lengthening with internal and external devices. J SurgOrthop Adv. 2015;24:174-179.
- Black S.R., Kwon M.S., Cherkshia A.M., et al. Lengthening in congenital femoral deficiency: a comparison of circular external fixation and a motorized intramedullary nail. J Bone Joint Surg Am. 2015;97:1432-1440.
- Fragomen AT. Transitioning to an intramedullary lengthening and compression nail. J Orthop Trauma. 2017;31:S7-S13.





 Journal of Orthopaedics Trauma Surgery and Related Research a publication of Polish Society, is a peer-reviewed online journal with quaterly print on demand compilation of issues published.
Journal of Orthopaedics Trauma Surgery and Related Research a publication of Polish Society, is a peer-reviewed online journal with quaterly print on demand compilation of issues published.