Periventricular leukomalacia
2 Assistant Professor, Department of Physiotherapy, Sports Research Lab, MMIPR MMU, Haryana, India, Email: pandey.aiims@gmail.com
Received: 19-Sep-2023, Manuscript No. jotsrr-23- 114246; Editor assigned: 21-Sep-2023, Pre QC No. jotsrr-23- 114246 (PQ); Accepted Date: Sep 29, 2023 ; Reviewed: 27-Sep-2023 QC No. jotsrr-23- 114246 (Q); Revised: 28-Sep-2023, Manuscript No. jotsrr-23- 114246 (R); Published: 30-Sep-2023
This open-access article is distributed under the terms of the Creative Commons Attribution Non-Commercial License (CC BY-NC) (http://creativecommons.org/licenses/by-nc/4.0/), which permits reuse, distribution and reproduction of the article, provided that the original work is properly cited and the reuse is restricted to noncommercial purposes. For commercial reuse, contact reprints@pulsus.com
Abstract
Periventricular leukomalacia is a white matter injury affecting the premature infant brain. PVL is a result from Hpoxia Ischemia (HI) with or without infection and is characterized by white matter necrotic lesions, hypomyelination and neural death.
Keywords
Periventricular leukomalacia, hypoxia ischemia
Introduction
Periventricular Leukomalacia (PVL) is a white matter injury affecting the premature infant brain. PVL is a result from Hypoxia Ischemia (HI) with or without infection and is characterized by white matter necrotic lesions, hypomyelination and neural death [1].
In the process of morphogenesis focuses PVL passes through 3 stages:
1. Necrosis: Death of cells or tissue through disease or injury. It occur when too little blood flows to the tissues. This can be from injury, radiations, or chemicals.
2. Resorption: It is the absorption that occur in the brain and increase the risk of brain damage and cause defects.
3. The formation gliosis scars or cysts: Cyst occur when large and confluent focuses, with mixed necrosis, in the centre and coagulation rim at the periphery.
Around the foci is generally defined area of lesions of the brain white matter the death of prooligodendrocytes, proliferation mikrogliocytesand astrocytes, swelling, bleeding, loss of capillaries. However, diffuse lesions without necrosis are not PVL.
PREVELANCE
The prevelance of PVL is seen worldwide and the incidence seen from range 19.8% to 34.1% and the range of cystic form is about 2.5% to 23% according to the researches.
In each year PVL affects about 20,000 to 30,000 children born prematurely who weigh less than 3.3 pounds whereas, 7000 of these children develop Cerebral Palsy (CP).
It is found that 75% affected children is preterm infants and upto 20% in term infants.
The PVL is most commonly happens between 23 to 20 weeks of gestation. After 24 weeks, there is axon and dendrites formation, differentiation synaptogenesi, myelination and synaptic pruning and developmental of circuitry.
This developmental process persists up to 2 years of age after birth.
WHITE MATTER
As it is a disease of white matter which is found in brain usually in deeper tissues of the brain (subcortical). It contain nerve fibers (axons) which are the extensions of nerve cells (neurons). Many of these nerve fibers are surrounded by a type of a sheath or covering called myelin. Whereas, myelin gives the white matter its color. As the white matter holds the capacity of solving problems and focus towards the work. It plays a crucial role in walking and balancing[2-4].
WHITE MATTER DISEASE STAGES
Lowest total WMSA (White Matter Signal Abnormality) (quartile 1, n=25)
Mid low total WMSA (quartile 2, n= 25)
Mid high total WMSA (quartile 3, n=25)
Highest total WMSA (quartile 4, n=22)
SYMPTOMS
Usually with the PVL babies it is seen that they do not generally have outward signs or symptoms of this disorder but they are at the risk for:
1. Motor disorder: These are the malfunctions of the nervous system that cause involuntary or uncontrollable movements or actions of the body. These disorders can cause lack of intended movements or an excess of involuntary movements.
2. Delayed cognitive development: It is a term used when a person has a certain limitations in mental functioning and in skills such as communicating, taking care of himself and herself and their social skills.
3. Co-ordination problem: In this a patient lost its control over the arms , legs and their posture and they are not able to respond as such over the commands .
4. Vision problem: In this the child is not able to fixed their gaze and focus over the thing with this they are not able to coordinate eye movements.
5. Hearing problem: It is the result of inner ear or nerve damage. This can range from mild to profound. It can be sensorineural, conductive, mixed and auditory neuropathy spectrum disorder.
6. Global Developmental Delay (GDD): It is typically presents a delay in multiple developmental areas. The areas may include speech, language, social, cognition, play and motor skills.
7. Mental and physical health disturbed: As in this all the GDD can be seen so the mental and physical fitness is reduced of PVL patients as they are not much engaged in activities.
8. Learning disability: The disorder that affect the ability to understand and response over that or use spoken or written language, do calculations and also defect in doing coordinate movements.
9. Seizures: A disorder in which nerve cell activity in the brain is disturbed and it is a result of genetic disorder or an acquired brain injury.
10. Spasticity: It is abnormal muscle tightness due to prolonged muscle contraction. It is a cause of damage of nerve pathways within the brain or spinal cord that control muscle movements.
11. Difficulty with eye movements: PVL can lead to defect in eye movement as it can associated with a cause of vision problem with the child. So, they are not able to focus or gaze an object constantly that can cause this issue.
12. Scoliosis: It is a sideway curvature of the spine. This is most often during the growth spurt just before puberty. In this the deformities can cause the change in posture.
13. Less social interaction: In this the child is less interactive with the society and do not respond accordingly.
14. Weakness: It is a lack of physical and muscle strength throughout the body which may result in generalized loss of efficiency to do the daily lifestyle activity.
INVESTIGATIONS
There are numerous investigations of PVL:
1. Cranial ultrasound: It is a painless test uses sound waves to view the baby’s brain through soft spot on the top of the head (fontanel). It is to evaluate the brain during the first year of life. It can detect the deformity in any part of the brain and is initial thing to do before any other investigation.
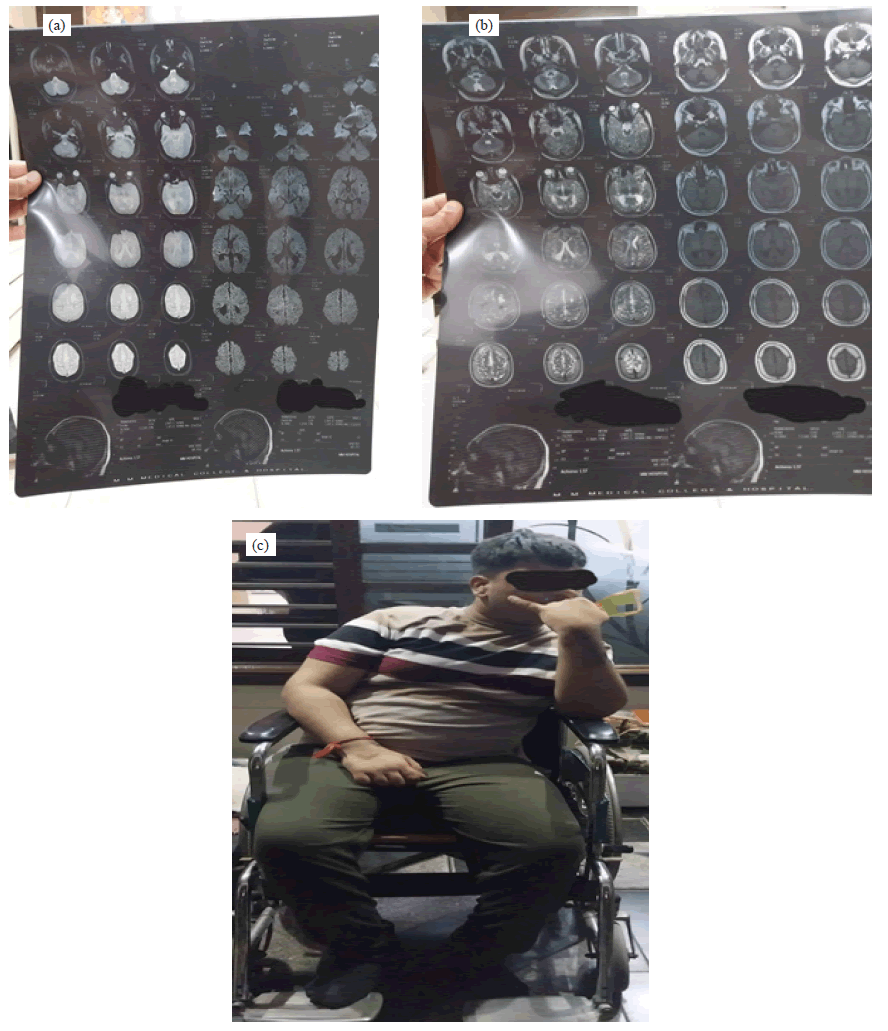
2. MRI (Magnetic Resonance Imaging): This imaging procedure uses a magnetic field and radio to produce a detailed picture of the brain without exposing the infant to X-rays. It is done in 1.5 T scanner, the routine protocol include conventional axial inversion recovery –weighted and T2-weighted imaging as well as diffusion weighted imaging. On the 3T scanner, the routine protocol include conventional 3D T1 and T2-weighted imaging (slice thickness 2 mm and T2 weighted TR 8670 ms).
3. CT (Computerized Tomography) SCAN: It is helpful to better evaluate the extent and severity of PVL. It may include ventriculomegaly involving the lateral ventricles with irregular margins of the ventricles and the loss of deep white matter. It is a series of x-ray images taken from different angles around the body and uses computer processing to create cross sectional images (slices) of the bones, blood vessels and soft tissues inside the body. It is the image of more detailed information than the plain x-ray. A CT can be used to examine the person who may have internal injuries or any other trauma. This can be used to visualize nearly all parts of the body and is used to diagnose disease or injury as well can ease to plan medical, surgical or radiation treatment [5-7].
Case Presentation
PATIENT’S DEMOGRAPHIC DATA
Name: Master XYZ
Age: 17 Year
Gender: Male
Address: UMNN
Chief Complaint: Patient was not able to blink the eyes from the birth itself and is not able to achieve the milestone at the time and not able to speak or recognize parents as well.
MANAGEMENT
1. Occupational Therapy (OT): It is a branch of health care that help people of all ages those who have physical, sensory or cognitive problems.This therapy helps with the people who is suffering from the barrier that is affecting their emotional, social and physical needs.
It is usually done for the kids and helps in the kids to play, improves their school performance and the daily living activities. It also boosts their confidence as well as their self-esteem and a sense of accomplishment Fig. 1.
It helps in develop fine motor skills, improves hand coordinations, masters basic life skills, learning of positive behavior, cognitive skills, sensory processing skills. Types,
2. Speech Therapy: It is the treatment that improves the ability to talk and use the language skills. It helps to express the thoughts and understand what others really want to convey to them so that they can improve the skills of memory and ability to solve problems by themselves. It can improve the early language skills, ability to use the voice, language comprehension, fluency, clarity and expressions.
This can solve the problem of cognitive communication disorders which include Dysarthria (that have slow and slurred speech. It can happen when the muscles that control speech become weak and the causes can be Multiple Sclerosis (MS), Amyotrophic Lateral Sclerosis (ALS) or any other nervous system disorder. Expressive disorders (person is not able to show up the thoughts), Fluency disorder (while speaking the person may feel the disrupt of speed, flow and rhythm), Resonance disorder (it affect the oral and nasal cavities), Receptive disorder (difficulty in comprehending or processing what other people say).
3. Re-education of the muscles: It is the technique to restore the normal body movements. It restore the nerves signals between the muscles and the brain for optimal function, which will be stored in the memory. As further it will help in attaining the normal movements for functioning ADLS (Activity of Daily Living) in a proper manner.
4. Physical Therapy (PT): It can help manage movement and reduce pain in individuals. According to APTA (American Physical Therapy Association) the physical therapy can improve range of motion, quality of life as well as prevent further injury or disability. It can improve mobility, movement, balance and fall prevention. As well as helps in avoiding or delay in surgery.
RISK FACTORS
1. Plancetal vascular anastomoses: In this the fetuses share a single planceta and vascular anastomoses on the fetal surface connects the blood circulation of both twins. There is a continuous exchange of blood between the twins.
2. Twin gestation: It means 2 fetus in the uterus. If there is PVL in the fetus then can lead to pre term birth of the babies which can lead Low Birth Weight (LBW).
3. Antepartum Hemorrhage (APH):- It is the bledding from or in to the genital tract, occurring from 24+0 weeks of pregnancy and prior to the birth of the birth. The main cause can be placental abruption, placental praevia and vasa praevia.
4. Chorioamnionitis and funitis: It is an acute inflammation of the membranes and chorion of the placenta. Typically due to ascending polymicrobial bacterial infection in the setting of membrane rupture.
DIFFERENTIAL DIAGNOSIS
1. Periventricular Venous Infarction: It is common in fetal stroke in which isolated subcortical injury may cause only motor deficits.
2. Cerebral Palsy: It is the abnormal brain development, often before birth. It is a congenital disorder of movement, muscle tone or posture.
3. White Matter Infract (WMS): It is a debilitating disorder which is characterized by the formation of ischemic lesions along subcortical white matter tracts of the central nervous system.
4. White Matter Gliosis: Cerebral cortical scarring/ gliosis can be caused by ischemic, infectious or traumatic processes. In prematurely born infants, the majority of gloitic lesions are encountered in the cerebral white matter which are usually not accomplished by epilepsy.
PREVENTION OF PVL
Children with PVL have a higher risk of developing cerebral palsy and for this medicos can take certain precautions to reduce the risk of PVL in pre- and full- term infants.
PVL PREVENTION METHOD INCLUDE:
1. Reducing the risk of prematurity
2. Preventing lack of oxygen / blood flow to the baby’s brain
3. Reducing blood pressure swings and hypotension
Conclusion
As there is no cure to PVL. Babies who have developed this should be in special care and with this therapies . As the decayed white matter in the brain will never regenerate and can not be repaired or restored. Although PVL is a permanent injury and the treatment can only helps the limitation in the progress of the disease.
References
- Reddy N, Doyle M, Hanagandi P, et al. Neuroradiological mimics of periventricular leukomalacia. J. Child Neurol.. 2022 Feb;37(2):151-67. [Google Scholar] [Cross ref]
- Romero-Guzman GJ, Lopez-Munoz F. Prevalence and risk factors for periventricular leukomalacia in preterm infants. A systematic review. Revista de neurologia. 2017 Jul 1;65(2):57-62. [Google Scholar] [Cross ref]
- Abiramalatha T, Bandyopadhyay T, Ramaswamy VV, et al. Risk factors for periventricular leukomalacia in preterm infants: a systematic review, meta-analysis, and GRADE-based assessment of certainty of evidence. Pediatr. Neurol. 2021 Nov;124:51-71. [Google Scholar] [Cross ref]
- Stefania P, Francesca T. Visual impairment and periventricular leukomalacia in children: A systematic review. Res. Dev. Disabil. 2023 Apr;135:104439. [Google Scholar] [Cross ref]
- Takashima S, Iida K, Deguchi K. Periventricular leukomalacia, glial development and myelination. Early hum. dev. 1995 Oct 2;43(2):177-84. [Google Scholar] [Cross ref]
- Roscigno CI. Periventricular leukomalacia: pathophysiological concerns due to immature development of the brain. J. Neurosci. Nurs. 2002 Dec;34(6):296-302. [Google Scholar] [Cross ref]
- Flodmark O, Roland EH, Hill A, et al. Periventricular leukomalacia: radiologic diagnosis. Radiology. 1987 Jan;162(1):119-24. [Google Scholar] [Cross ref]



 Journal of Orthopaedics Trauma Surgery and Related Research a publication of Polish Society, is a peer-reviewed online journal with quaterly print on demand compilation of issues published.
Journal of Orthopaedics Trauma Surgery and Related Research a publication of Polish Society, is a peer-reviewed online journal with quaterly print on demand compilation of issues published.